Maintaining optimal bone integrity is crucial not only for mobility and quality of life but also for mitigating risks associated with various chronic ailments. Bone tissue functions as a dynamic organ that continuously remodels in response to physiological stimuli, nutritional intake, and systemic health factors. When chronic diseases such as Diabetes Mellitus or Rheumatoid Arthritis are present, complex interactions between inflammatory cascades, hormonal imbalances, and lifestyle factors can accelerate bone loss and compromise skeletal resilience. This article explores the underlying mechanisms, diagnostic modalities, and comprehensive management strategies designed to preserve bone health within the context of chronic disease care.
Pathophysiology of Bone Deterioration in Chronic Diseases
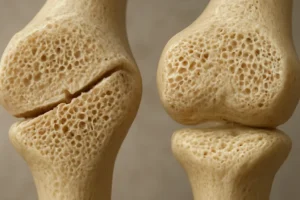
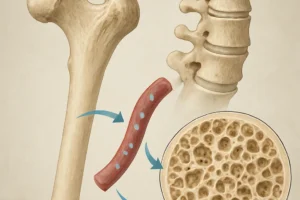
Bone remodeling relies on a delicate equilibrium between osteoblast-mediated formation and osteoclast-driven resorption. Chronic inflammatory disorders disrupt this balance by promoting excessive osteoclast activity and inhibiting osteoblast function. Elevated cytokines such as interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-α) induce osteoclastogenesis and reduce bone mineral density, setting the stage for osteoporosis and increased fracture risk.
Inflammatory Processes
Systemic inflammation represents a pivotal driver of bone loss. In conditions like Psoriatic Arthritis or inflammatory bowel diseases, proinflammatory mediators upregulate receptor activator of nuclear factor κB ligand (RANKL), favoring bone resorption. Simultaneously, oxidative stress impairs osteoblast viability, further skewing remodeling dynamics. Chronic inflammation can also impair vascular supply to bone, compromising the delivery of nutrients essential for matrix synthesis.
Nutritional and Hormonal Deficiencies
Chronic kidney disease (CKD) often precipitates disturbances in mineral homeostasis, notably calcium and phosphate imbalances, as well as vitamin D deficiency. Secondary hyperparathyroidism arises when parathyroid hormone levels escalate to compensate for low serum calcium, thereby intensifying bone turnover. Malabsorptive syndromes associated with celiac disease or post-bariatric surgery may lead to insufficient absorption of calcium and vitamin D, further jeopardizing bone strength.
Diagnostic and Monitoring Strategies
Early detection of compromised bone health facilitates timely interventions that can arrest or reverse pathological remodeling. A multifaceted diagnostic approach encompasses imaging, biochemical markers, and functional assessments to gauge bone integrity and fracture risk.
Imaging Modalities
Dual-energy X-ray absorptiometry (DXA) remains the gold standard for quantifying bone mineral density and diagnosing osteopenia or osteoporosis. High-resolution peripheral quantitative computed tomography (HR-pQCT) offers three-dimensional insights into trabecular architecture and cortical thickness, enhancing risk stratification in patients with chronic inflammatory diseases.
Biochemical Markers and Clinical Tools
Bone turnover markers such as serum C-terminal telopeptide (CTX) and procollagen type I N-terminal propeptide (P1NP) reflect resorption and formation rates, respectively. Incorporating these measurements into clinical practice allows for monitoring therapeutic responsiveness. Risk assessment algorithms like FRAX integrate clinical risk factors with BMD values to estimate ten-year fracture probability, guiding personalized management plans.
Integrated Management Approaches
Optimal care of bone health in patients with chronic disease demands a synergistic strategy that combines pharmacotherapy, lifestyle modifications, nutrition optimization, and rehabilitation. Interdisciplinary collaboration among rheumatologists, endocrinologists, dietitians, and physical therapists is essential to achieve comprehensive outcomes.
Pharmacological Interventions
Anti-resorptive agents such as bisphosphonates inhibit osteoclast-mediated bone loss and have a well-established role in preventing fragility fractures. Denosumab, a monoclonal antibody against RANKL, offers an alternative for patients intolerant to bisphosphonates. In cases of severe osteoporosis, anabolic therapies like teriparatide stimulate osteoblast activity to rebuild bone mass. Sequential or combination regimens should be tailored according to individual risk profiles and comorbid conditions.
Lifestyle and Nutritional Support
Weight-bearing and resistance exercises enhance skeletal loading, stimulating bone formation through mechanotransduction pathways. Balance training reduces fall risk, thereby preventing fractures. Adequate dietary intake of calcium (1,000–1,200 mg daily) and vitamin D (800–1,000 IU daily) is vital for mineralization and muscle function. Supplementation may be necessary when dietary sources are insufficient or in the presence of malabsorption. Lifestyle factors such as smoking cessation and moderation of alcohol intake further contribute to bone preservation.
Physical Rehabilitation and Fall Prevention
Customized physiotherapy regimens address mobility limitations and muscle weakness, common in patients with chronic illnesses. Gait analysis and home safety evaluations identify environmental hazards, while assistive devices mitigate the impact of balance impairments. Educating patients on safe movement strategies fosters self-efficacy and reduces the incidence of falls.
Emerging Research and Future Perspectives
Advancements in molecular biology have unveiled novel targets for modulating bone metabolism. Investigational agents such as sclerostin inhibitors demonstrate promise in enhancing bone formation by antagonizing the Wnt signaling pathway. Regenerative medicine approaches, including mesenchymal stem cell therapies, aim to restore osteogenic potential in severely compromised bone. Biomaterial scaffolds impregnated with growth factors offer innovative platforms for localized bone regeneration following fracture or surgical interventions.
In parallel, digital health technologies are transforming patient monitoring and adherence. Wearable sensors can track physical activity levels, gait patterns, and even detect early signs of falls. Telemedicine platforms facilitate remote consultations, enabling timely adjustments to treatment protocols and reinforcing patient engagement. As personalized medicine evolves, genomics and proteomics may yield predictive markers for bone fragility, guiding preemptive strategies tailored to each patient’s genetic and molecular profile.
Comprehensive management of bone health in the setting of chronic disease requires an integrated, evidence-based approach. By combining targeted therapies with nutritional, rehabilitative, and technological innovations, healthcare providers can significantly enhance skeletal resilience and overall quality of life for affected individuals.