The interplay between the gastrointestinal tract and skeletal system is a critical aspect of overall health. In patients with celiac disease, the immune-mediated damage to the small intestine can lead to significant consequences for bone mineral density and increase the risk of osteoporosis. Understanding the mechanisms, assessment strategies, and management approaches is essential for clinicians and patients alike.
Background and Pathophysiology
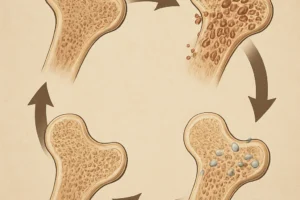
Celiac disease is an autoimmune condition triggered by ingestion of gluten, which causes inflammation and villous atrophy in the small intestine. This damage impairs the absorption of key nutrients such as calcium and vitamin D, both crucial for bone health. Chronic malabsorption leads to secondary hyperparathyroidism, accelerating bone resorption and reducing bone formation.
Immune-Mediated Intestinal Injury
- Exposure to gluten peptides activates an immunological response mediated by tissue transglutaminase.
- Proinflammatory cytokines such as interleukin-15 contribute to enterocyte apoptosis and villous blunting.
- Loss of villi area decreases the absorptive surface, leading to nutritional deficiencies.
Consequences for Bone Metabolism
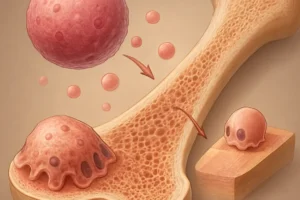
- Decreased serum calcium stimulates parathyroid hormone (PTH) release, promoting bone resorption.
- Insufficient vitamin D conversion in enterocytes undermines calcium homeostasis.
- Chronic inflammation may have direct effects on osteoblast and osteoclast activity, tipping the balance toward bone loss.
Clinical Presentation and Diagnosis
Bone-related manifestations in celiac patients range from asymptomatic reductions in bone density to overt fractures. Early detection of bone involvement is critical to prevent long-term morbidity.
Signs and Symptoms
- Non-specific musculoskeletal pain, often described as diffuse back or joint discomfort.
- Height loss or kyphosis in advanced osteoporosis.
- Fragility fractures, particularly of the vertebrae, hip, and wrist.
- Fatigue and muscle weakness related to vitamin D deficiency.
Diagnostic Workup
Screening and confirmatory testing should include:
- Serologic tests: Tissue transglutaminase IgA and endomysial antibodies.
- Small-bowel biopsy demonstrating villous atrophy and crypt hyperplasia.
- Dual-energy X-ray absorptiometry (DEXA) to quantify bone mineral density.
- Laboratory evaluation of serum calcium, phosphate, PTH, 25-hydroxyvitamin D, and markers of bone turnover.
Management Strategies
Effective intervention requires a multidisciplinary approach that targets both the underlying intestinal damage and the associated bone disease.
Gluten-Free Diet
- Strict adherence to a gluten-free diet is the cornerstone of therapy, allowing intestinal healing and improved nutrient absorption.
- Nutritional counseling is essential to avoid hidden sources of gluten and ensure adequate calorie intake.
- Regular follow-up of serologic markers helps assess dietary compliance and mucosal recovery.
Supplementation and Pharmacotherapy
To counteract deficiencies and support bone health, consider:
- Calcium supplementation (1200–1500 mg/day) divided doses to enhance absorption.
- Vitamin D3 supplementation (800–2000 IU/day), adjusted based on 25-hydroxyvitamin D levels.
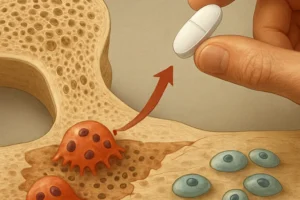
- Bisphosphonates for patients with osteoporosis or high fracture risk, to inhibit osteoclast-mediated bone resorption.
- Emerging therapies such as denosumab or teriparatide may be indicated in refractory cases.
Lifestyle and Supportive Measures
- Weight-bearing exercises to stimulate bone formation and improve muscle strength.
- Smoking cessation and moderation of alcohol intake, both known risk factors for bone loss.
- Fall prevention strategies, including home safety assessments and balance training.
- Regular monitoring of bone density every 1–2 years in high-risk individuals.
Special Considerations and Future Directions
Continued research is illuminating the complex links between immune function, gut integrity, and bone metabolism. Novel biomarkers and imaging techniques may enable earlier detection of bone compromise.
Non-Classical Presentation
- Some patients exhibit bone loss without significant gastrointestinal symptoms, underscoring the importance of screening in atypical cases.
- Seronegative celiac disease may require HLA typing or trial of a gluten-free diet to confirm diagnosis.
Microbiome and Bone Health
- Alterations in gut microbiota composition may influence calcium absorption and immune regulation.
- Probiotics and prebiotics are under investigation for potential adjunctive benefits to bone density.
Personalized Medicine
- Genetic profiling could help predict severity of bone involvement and guide therapy intensity.
- Pharmacogenomic approaches may optimize bisphosphonate or biologic treatment selection.