Advances in bone fracture fixation devices have revolutionized the field of orthopedics by enhancing stability, accelerating healing, and reducing complications. This comprehensive article explores the evolution, cutting-edge materials, biomechanical principles, clinical innovations, and future perspectives in fracture fixation, highlighting the multidisciplinary approaches that shape modern patient care.
History and Evolution of Fixation Techniques
The journey of mechanical stabilization of broken bones commenced centuries ago, when rudimentary splints and wooden splints provided basic support. Over time, the introduction of metal plates and screws marked a significant transformation. Early pioneers experimented with steel implants, which offered improved stability but often faced issues related to infection and implant failure. The mid-20th century witnessed the widespread adoption of compression plates and intramedullary nails, setting the stage for today’s sophisticated devices.
Key historical milestones:
- The AO (Arbeitsgemeinschaft für Osteosynthesefragen) principles, established in the 1950s, formalized guidelines for anatomical reduction, stable fixation, and early mobilization.
- Development of low-profile plates minimized soft tissue irritation and emphasized periosteal blood supply preservation.
- Introduction of locking plates in the 1990s enhanced the mechanical interface between screws and plates, especially beneficial in osteoporotic bone.
Modern Materials and Design Innovations
Titanium Alloys and Biocompatibility
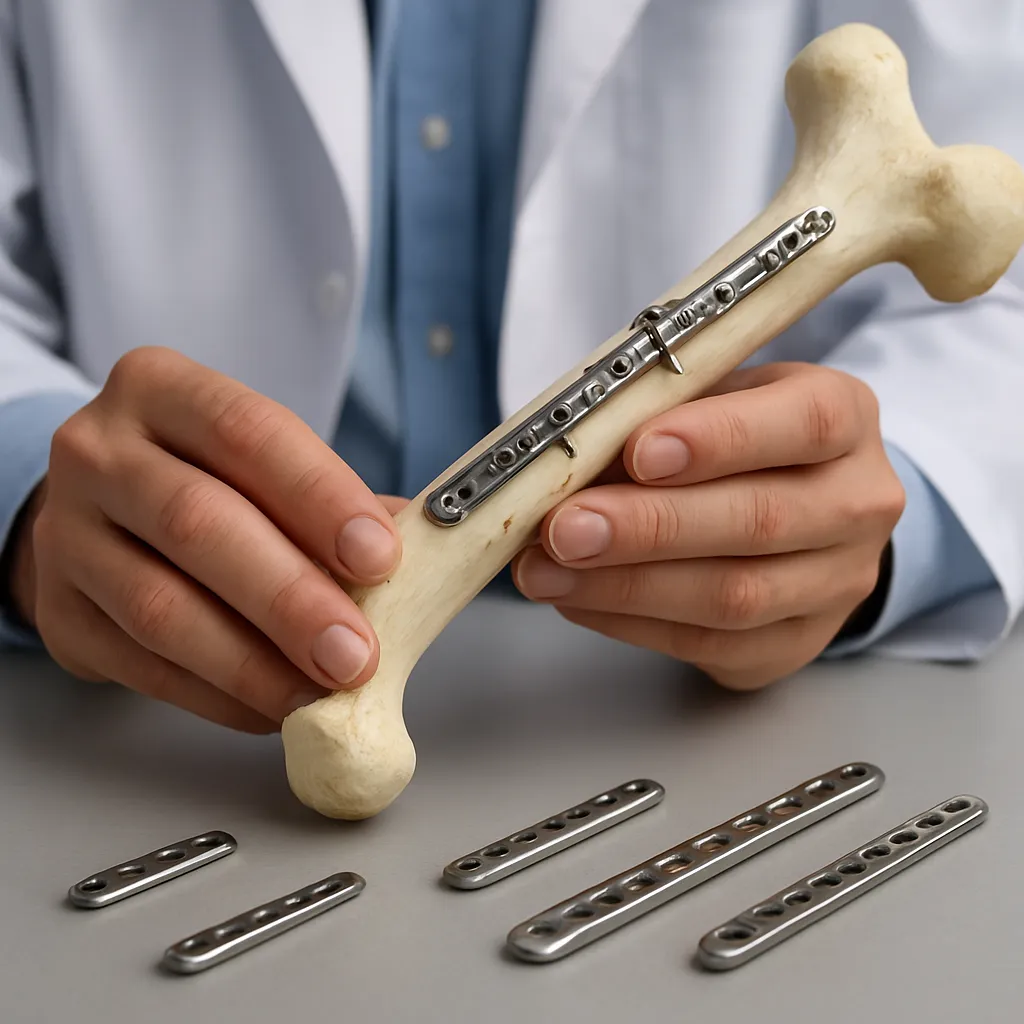
Titanium and its alloys stand at the forefront due to their excellent biocompatibility, corrosion resistance, and favorable strength-to-weight ratio. The elastic modulus of titanium more closely matches that of cortical bone, reducing stress shielding and promoting natural load transfer. Customizable geometry achieved through computer-aided design (CAD) enables contouring to complex anatomies.
Biodegradable Polymers and Resorbable Devices
Resorbable fixation systems composed of polylactic acid (PLA), polyglycolic acid (PGA), or magnesium-based alloys offer temporary support that gradually degrades as the bone heals. This innovation eliminates the need for secondary surgery to remove hardware. Critical considerations include controlled degradation rates, mechanical integrity throughout the healing period, and byproduct biocompatibility.
Smart and Bioactive Coatings
Integration of bioactive coatings, such as hydroxyapatite or antimicrobial silver nanoparticles, seeks to enhance osseointegration and reduce infection risk. Emerging smart coatings may deliver growth factors or antibiotics in response to physiological triggers, thereby combining mechanical support with targeted biological therapy.
Biomechanical Principles Underpinning Device Performance
Effective fracture fixation demands meticulous attention to biomechanics. Optimal devices distribute load across the fracture site, prevent micromotion beyond tolerable thresholds, and maintain alignment under physiological stresses. Finite element analysis (FEA) has become indispensable for simulating implant behavior under various load scenarios, guiding both material selection and structural design.
- Load Sharing vs. Load Bearing: Plates can function in a load-sharing capacity when combined with adequate callus formation, whereas intramedullary nails often assume a load-bearing role in specific fracture patterns.
- Screw-Plate Interface: Locking mechanisms prevent toggle and pull-out in osteoporotic bone, safeguarding fixation in high-risk patient populations.
- Stress Shielding: Implants with excessive stiffness divert load away from bone, potentially compromising remodeling. Tailoring elasticity mitigates this phenomenon.
Clinical Applications and Procedural Advances
Contemporary fracture fixation extends beyond simple plating and nailing. Minimally invasive techniques, image-guided navigation, and three-dimensional (3D) printing have broadened the therapeutic arsenal.
- Minimally Invasive Plate Osteosynthesis (MIPO): Small incisions preserve blood supply and soft tissue integrity, reducing wound complications and facilitating early mobilization.
- Intraoperative Navigation: Real-time imaging and augmented reality improve screw placement accuracy, particularly in complex pelvic and spinal fractures.
- 3D-Printed Patient-Specific Implants: Customized plates and jigs, derived from preoperative CT scans, ensure perfect conformity to anatomical contours and can address irregular fractures or bone defects.
Notable clinical studies demonstrate that combining innovation in implant design with enhanced surgical techniques yields superior functional outcomes, faster rehabilitation, and lower rates of nonunion.
Emerging Technologies and Future Perspectives
Looking ahead, the convergence of material science, regenerative medicine, and digital technologies promises groundbreaking developments in fracture management.
- Bioinspired Polymers: Mimicking bone’s hierarchical structure, these materials can dynamically adjust stiffness and support progressive callus maturation.
- Stem Cell–Loaded Scaffolds: Incorporating mesenchymal stem cells into fixation constructs may actively promote osteogenesis, accelerating union in challenging fractures.
- Embedded Sensors: ‘Smart’ implants with strain gauges or microelectromechanical systems (MEMS) could monitor healing metrics, providing clinicians with objective data to tailor weight-bearing protocols.
- Robotic-Assisted Fixation: Robotics enhance precision and reproducibility in implant placement, particularly beneficial in anatomically complex regions or when extreme accuracy is paramount.
Ongoing research emphasizes the translation of laboratory innovations into clinically viable products, balancing strength, flexibility, and safety. Collaborative efforts between engineers, surgeons, and material scientists remain pivotal in ushering the next era of fracture fixation excellence.