Bone health in individuals suffering from eating disorders represents a critical intersection between nutritional status, endocrine function, and skeletal integrity. This article delves into the mechanisms by which disordered eating, such as anorexia nervosa and bulimia nervosa, compromises bone strength and elevates fracture risk. Through examination of underlying pathophysiology, diagnostic strategies, and therapeutic interventions, clinicians can better address this often-overlooked complication and improve long-term outcomes for affected patients.
Pathophysiology of Bone Loss
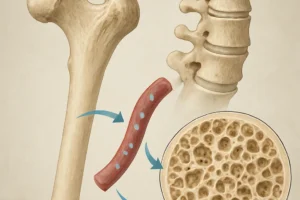
Bone is a dynamic tissue regulated by the continuous interplay of osteoblast-mediated formation and osteoclast-driven resorption. In patients with eating disorders, several factors disrupt this homeostasis, leading to reduced bone density and structural deterioration.
Energy Deficiency and Hormonal Imbalances
- Malnutrition: Prolonged calorie restriction diminishes the substrates necessary for collagen synthesis and mineralization.
- Estrogen deficiency: In anorexia nervosa, amenorrhea leads to hypoestrogenism, which is strongly correlated with accelerated bone resorption and loss of trabecular bone.
- Altered levels of leptin, ghrelin, and insulin-like growth factor 1 (IGF-1) further impair osteoblast activity.
Secondary Endocrine Effects
Chronic undernutrition and stress-induced hypercortisolemia generate a catabolic milieu:
- Elevated cortisol stimulates osteoclastogenesis and inhibits bone formation.
- Thyroid hormone abnormalities, often subclinical, can enhance bone turnover.
- Growth hormone resistance reduces the anabolic impact of IGF-1 on the skeleton.
Microarchitectural Alterations
Beyond quantitative losses, eating disorders provoke qualitative changes in bone structure:
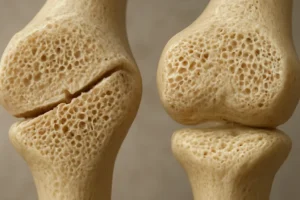
- Trabecular thinning and perforation compromise mechanical strength.
- Cortical porosity increases, further weakening load-bearing capacity.
- Irregular mineralization patterns are observed under histological examination, indicative of impaired remodeling.
Clinical Assessment and Imaging
Early recognition of skeletal involvement is paramount. A thorough evaluation combines clinical history, physical examination, and targeted imaging studies.
Risk Factor Identification
- Duration and severity of restrictive eating behaviors.
- History of amenorrhea or menstrual irregularities in female patients.
- Previous low-trauma fracture risk events.
Biochemical Markers
- Bone turnover markers, such as serum C-terminal telopeptide (CTX) and procollagen type 1 N-terminal propeptide (P1NP), reveal increased resorption and decreased formation.
- Nutritional indices: albumin, prealbumin, and vitamin D levels inform overall nutritional status.
- Hormonal panels assess estrogen, cortisol, thyroid, and IGF-1 concentrations.
Imaging Modalities
The gold standard for diagnosing low bone mass is dual-energy X-ray absorptiometry (DXA). It quantifies areal bone mineral density (BMD) at the lumbar spine, hip, and forearm. However, emerging techniques offer deeper insights:
- High-resolution peripheral quantitative computed tomography (HR-pQCT) evaluates microarchitectural detail.
- Trabecular bone score (TBS) derived from DXA images reflects trabecular integrity.
- Quantitative ultrasound (QUS) provides a radiation-free alternative for peripheral sites.
Management Approaches
Optimal treatment of bone disease in eating disorders requires a multidisciplinary strategy, blending nutritional rehabilitation, hormonal optimization, and targeted pharmacotherapy.
Nutritional Rehabilitation
- Gradual caloric repletion is essential to restore lean body mass without precipitating refeeding syndrome.
- Macronutrient balance, emphasizing adequate protein intake, supports matrix synthesis.
- Supplementation with calcium and vitamin D addresses common deficiencies and promotes mineralization.
Endocrine Therapies
- In amenorrheic women, physiologic transdermal or low-dose oral estrogen can improve BMD, though combined progesterone is required to protect the endometrium.
- Testosterone replacement in hypogonadal men may benefit bone mass, albeit evidence is less robust.
- Recombinant IGF-1 has shown promise in select trials by enhancing bone formation markers.
Pharmacological Interventions
Drug therapy is considered when nutritional and hormonal measures prove insufficient, or when fracture risk persists elevated:
- Bisphosphonates: These antiresorptive agents reduce osteoclast activity but warrant caution in women of childbearing potential due to long half-life.
- Denosumab: A monoclonal antibody against RANKL that inhibits bone resorption; useful in cases intolerant to bisphosphonates.
- Teriparatide: An anabolic parathyroid hormone analog reserved for severe osteoporosis, with strict treatment duration limits.
Future Directions and Research
Advances in understanding bone pathology in eating disorders point to novel therapeutic targets and diagnostic tools. Researchers are exploring:
- Selective estrogen receptor modulators (SERMs) that mimic estrogen’s skeletal benefits without reproductive side effects.
- Wnt signaling pathway modulators to enhance osteoblast differentiation and survival.
- Noninvasive biomarkers, such as circulating microRNAs, that predict bone loss earlier than conventional methods.
By integrating cutting-edge research with comprehensive clinical care, the medical community can better preserve skeletal health and reduce the long-term morbidity associated with eating disorders.