The widespread use of antidepressants has raised important questions about their long-term effects beyond mood regulation. Recent research suggests that these medications may influence bone density and structural integrity, potentially altering the risk of fractures and osteoporosis. This article examines the complex interplay between commonly prescribed antidepressants and bone health, detailing underlying mechanisms, clinical evidence, and management strategies to help clinicians and patients navigate these concerns.
Understanding the Relationship Between Antidepressants and Bone Health
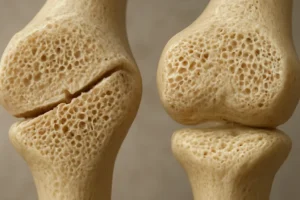
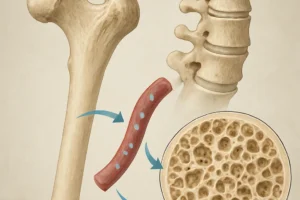
Antidepressants, particularly selective serotonin reuptake inhibitors (SSRIs) and tricyclic compounds, are among the most frequently prescribed medications worldwide. While they effectively treat depression and anxiety disorders, mounting evidence indicates that prolonged use may negatively impact the skeleton. Bone is a dynamic tissue constantly undergoing remodeling: old bone is resorbed by osteoclasts, whereas osteoblasts form new bone. Any interference with this balance can lead to decreased bone strength and increased susceptibility to fracture risk.
Several observational studies have linked chronic SSRI therapy to reductions in bone mineral density (BMD), particularly in older adults. This association underscores the significance of understanding how antidepressants modulate bone metabolism and what factors—such as age, sex, and concurrent medical conditions—may exacerbate vulnerability. Patients and clinicians should be aware that the benefits of improved mental health must be weighed against potential skeletal side effects in susceptible populations.
Biological Mechanisms Impacting Bone Remodeling
Serotonin Signaling Pathway
Serotonin is a critical neuromodulator in the brain, but it also plays an essential role in peripheral tissues, including bone. Osteoblasts and osteoclasts express serotonin receptors and transporters that regulate local serotonin concentrations. SSRIs inhibit the serotonin transporter (SERT), leading to elevated extracellular serotonin. While increased central serotonin alleviates depressive symptoms, peripheral accumulation can:
- Enhance osteoclast activity, accelerating bone resorption.
- Inhibit osteoblast proliferation, impairing bone formation.
- Alter expression of bone-specific growth factors, such as RANKL and OPG.
These disruptions to the finely tuned remodeling cycle may cumulatively reduce bone mass over time.
Hormonal and Metabolic Effects
Beyond serotonin pathways, antidepressants can influence endocrine and metabolic factors crucial for skeletal integrity. Chronic exposure to certain drugs may dysregulate the hypothalamic-pituitary-adrenal (HPA) axis, raising circulating cortisol levels. Elevated cortisol is known to promote bone resorption and suppress collagen synthesis. Additionally, some antidepressants interfere with vitamin D metabolism, lowering active vitamin D levels necessary for calcium absorption. Combined with reduced appetite and nutritional intake often seen in depression, these hormonal changes can exacerbate bone loss and weaken structural resilience.
Clinical Evidence and Epidemiological Findings
Clinical and population-based studies have provided mixed results regarding the magnitude of bone changes associated with antidepressant use. Key findings include:
- Longitudinal cohorts report a 5–10% decline in hip and lumbar spine BMD after ≥2 years on SSRIs.
- Meta-analyses indicate a 1.2- to 1.8-fold increase in osteoporosis incidence among long-term SSRI users compared to non-users.
- Women, especially postmenopausal, appear more vulnerable to medication-induced bone changes due to lower baseline estrogen levels.
- Tricyclic antidepressants (TCAs) show weaker associations with BMD loss but may contribute to falls through sedation and orthostatic hypotension.
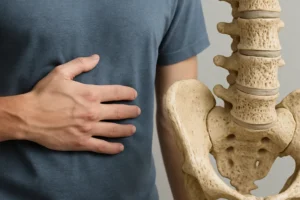
Fracture registries further confirm that patients on SSRIs have a modestly increased risk of wrist, hip, and vertebral fractures. While the absolute risk remains relatively low for young adults, older individuals and those with preexisting osteoporosis face a significantly higher threat.
Strategies for Patient Management and Risk Mitigation
Monitoring Bone Health
Early identification of at-risk individuals is crucial. Recommended monitoring steps include:
- Baseline dual-energy X-ray absorptiometry (DXA) scans before initiating long-term antidepressant therapy.
- Periodic reassessment of BMD (every 1–2 years) to detect accelerated bone loss.
- Laboratory tests for vitamin D, calcium, and markers of bone turnover when clinically indicated.
- Fall-risk assessments, particularly in elderly patients, to address modifiable hazards.
Pharmacological Alternatives and Supplementation
When bone health concerns arise, clinicians may consider:
- Switching to antidepressants with a lower impact on bone metabolism, such as bupropion or certain atypical agents.
- Initiating antiresorptive therapies (e.g., bisphosphonates, denosumab) in high-risk patients.
- Ensuring adequate supplementation with calcium (1,000–1,200 mg/day) and vitamin D (800–2,000 IU/day).
- Encouraging regular weight-bearing and muscle-strengthening exercises to promote bone formation.
Collaborative care involving psychiatrists, endocrinologists, and primary care providers can optimize both mental health treatment and skeletal preservation.
Emerging Research and Future Directions
Ongoing investigations aim to refine our understanding of how different classes of antidepressants interact with bone remodeling at molecular and clinical levels. Novel areas of interest include the role of microbiome alterations on bone metabolism, pharmacogenomic predictors of skeletal sensitivity, and development of targeted therapies that minimize peripheral serotonin effects. Personalized approaches to mental health treatment may eventually allow clinicians to tailor antidepressant choice based on an individual’s genetic risk profile for osteoporosis, optimizing outcomes across multiple physiological systems.