Regular engagement in targeted exercise routines plays a pivotal role in maintaining optimal bone density and reducing the likelihood of developing osteoporosis. By understanding how different forms of physical activity deliver beneficial mechanical stress to the skeletal system, healthcare professionals and individuals alike can craft personalized regimens aimed at strengthening the bones, improving balance, and ultimately lowering fracture risk.
Mechanical Stimuli and Bone Remodeling
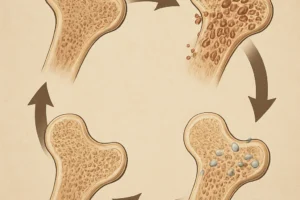
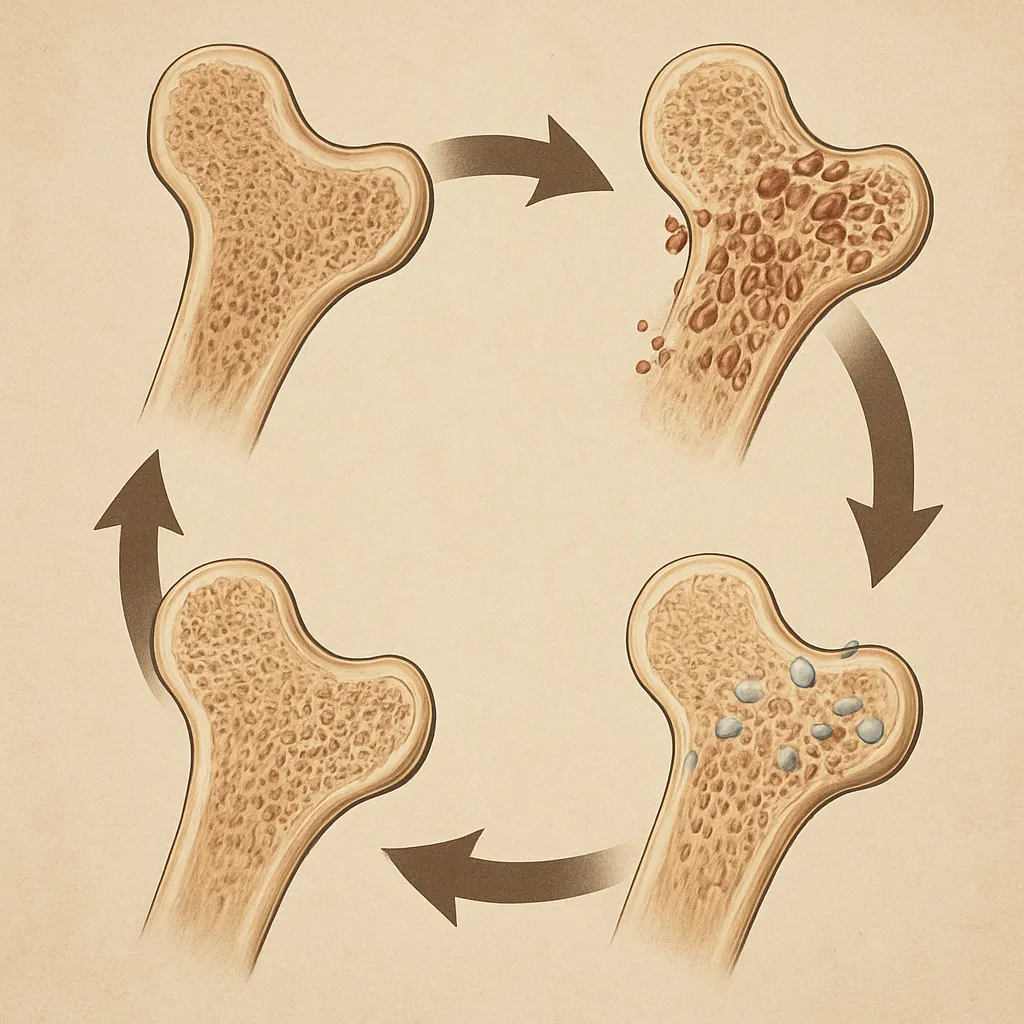
Bone is a dynamic tissue that responds to its mechanical environment. Wolff’s Law describes how bones adapt over time: when exposed to increased load or tension, bone-forming cells (osteoblasts) become more active. Conversely, in the absence of load, bone-resorbing cells (osteoclasts) dominate, leading to net bone loss. This constant turnover cycle is known as remodeling. Key factors in this process include the magnitude, rate, and frequency of mechanical signals delivered by weight-bearing movement.
Mechanotransduction Pathways
Mechanotransduction involves converting mechanical forces into cellular responses. Strain on the bone matrix triggers ion channels on osteocyte membranes, releasing signaling molecules that orchestrate remodeling. The interplay between sclerostin, produced by osteocytes, and the Wnt/β-catenin pathway promotes osteoblast proliferation when sclerostin levels drop under load-bearing activities.
Influence of Hormonal Regulation
Physical activity also modulates hormonal regulation relevant to bone health. Exercise stimulates growth hormone and insulin-like growth factor 1 (IGF-1), both of which encourage bone formation. In addition, regular activity promotes sensitivity to sex steroids such as estrogen and testosterone, essential for maintaining bone mass, especially in aging populations.
Types of Beneficial Exercises
Selecting the right modalities is crucial for maximizing skeletal benefits. The following categories of exercise have been extensively studied for their osteoprotective effects.
- Weight-Bearing Aerobics: Activities such as brisk walking, jogging, and stair climbing force bones to work against gravity. The vertical impact generates compressive forces that stimulate bone adaptation.
- Resistance Training: Lifting weights or using resistance bands applies tension through muscle contractions, encouraging increased bone mineral content. Common exercises include squats, lunges, and chest presses.
- High-Impact Activities: Jumping, hopping, and skipping can be introduced cautiously to create dynamic loads. Such sinusoidal stress patterns produce rapid peaks that strongly activate osteogenic signaling.
- Balance and Functional Exercises: Tai chi, yoga, and targeted stability drills reduce fall risk by improving proprioception, gait, and muscle coordination. These indirect benefits complement direct bone-strengthening effects.
- Whole-Body Vibration: Platforms delivering low-amplitude vibrations encourage mechanotransduction in weight-bearing bones. Short daily sessions have shown promise in clinical trials, particularly for those unable to perform traditional high-impact movements.
Exercise Programming Considerations
Intensity, duration, and progression must be tailored to individual fitness levels, existing bone health, and comorbidities. A typical regimen might include three weekly sessions mixing resistance sets with 20–30 minutes of weight-bearing cardio. Adequate rest between high-impact days prevents overuse injuries and allows remodeling processes to consolidate gains.
Special Considerations and Guidelines
Prevention strategies should account for life stages, nutritional status, and underlying medical conditions.
Postmenopausal Women
Estrogen deficiency accelerates bone resorption, elevating osteoporosis risk. Integrating progressive resistance training and targeted high-impact moves can attenuate this rapid decline. Monitoring vitamin D levels enhances calcium absorption, ensuring that mechanical stimuli translate into mineral deposition.
Individuals with Low Baseline Fitness or Frailty
For those newly embarking on an exercise program, beginning with low-intensity weight-bearing and balance drills is essential. As strength and confidence develop, incremental increases in resistance and impact help promote continuous adaptation without excessive injury risk.
Nutrition and Lifestyle Synergy
Exercise represents one pillar of bone health. Adequate daily intake of calcium and vitamin D supports the biological processes triggered by mechanical load. Avoidance of smoking and moderation of alcohol consumption protect against inflammation and hormonal imbalances that undermine bone integrity.
Monitoring and Assessment
Dual-energy X-ray absorptiometry (DXA) scans provide baseline and follow-up values for bone mineral density (BMD). Periodic assessments guide exercise intensity adjustments. Clinicians may also track markers of bone turnover in blood or urine to evaluate biochemical responses to training.
By harnessing the principles of biomechanics, endocrinology, and tailored programming, structured exercise regimens serve as a powerful defense against the gradual decline in skeletal strength that characterizes osteoporosis. Interdisciplinary approaches combining physical activity with nutrition and medical oversight create the most robust framework for preserving bone health across the lifespan.