Phosphorus plays a pivotal role in maintaining optimal bone integrity and overall skeletal health. As the second most abundant mineral in the human body, it participates in a variety of physiological processes that extend beyond simply providing structural support. This article explores the multifaceted functions of phosphorus in the context of bone biology and medicine, highlighting the critical balance required to preserve mineralization, regulate metabolism, and prevent common disorders such as rickets and osteoporosis.
Importance of Phosphorus in Skeletal Structure
Within the matrix of bone tissue, phosphorus combines with calcium to form hydroxyapatite crystals, which give bones their strength and rigidity. Approximately 85% of the body’s phosphorus resides in this mineralized matrix, providing a reservoir essential for maintaining homeostasis of critical ions in the bloodstream.
Hydroxyapatite Formation
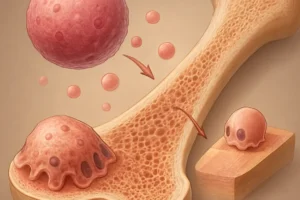
Bone is composed of an organic collagen framework and an inorganic mineral phase. The inorganic component primarily consists of calcium phosphate in the form of hydroxyapatite (Ca10(PO4)6(OH)2). During bone mineralization, osteoblasts secrete matrix vesicles that serve as nucleation centers for crystal growth. Phosphorus ions accumulate within these vesicles and interact with calcium to initiate the formation of robust crystals.
Structural Integrity and Load Bearing
The unique architecture provided by hydroxyapatite crystals allows bones to withstand mechanical stress and distribute loads without fracturing. A deficiency or imbalance in phosphorus can compromise the quality and density of this mineral phase, making bones more susceptible to fractures and deformities.
Metabolic Pathways and Nutrient Interactions
Phosphorus is not only a structural component but also central to numerous metabolic pathways. It contributes to energy metabolism, cell signaling, and acid-base balance, all of which indirectly affect bone health.
Energy Metabolism and ATP Production
- Adenosine triphosphate (ATP) contains three phosphate groups and serves as the primary energy currency for cellular processes.
- During hydrolysis of ATP, inorganic phosphate is released, fueling osteoblastic activity and bone formation.
Hormonal Regulation and Mineral Balance
Phosphorus homeostasis is regulated by a triad of hormones:
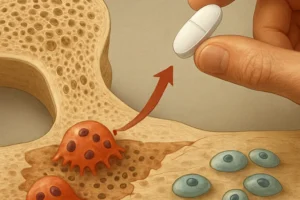
- Parathyroid hormone (PTH): Increases renal excretion of phosphorus while promoting calcium reabsorption, indirectly stimulating bone resorption when serum calcium is low.
- Fibroblast growth factor 23 (FGF23): Secreted by osteocytes, it reduces renal phosphate reabsorption and vitamin D activation.
- Vitamin D (Calcitriol): Enhances intestinal absorption of both calcium and phosphorus, facilitating bone mineralization.
Disruption in any of these pathways can result in imbalanced serum phosphorus levels, leading to conditions such as hyperphosphatemia or hypophosphatemia, each carrying its own risk profile for skeletal health.
Dietary Sources and Recommendations
Optimal phosphorus intake is essential to support bone remodeling and prevent metabolic bone diseases. It is important to consider both dietary sources and potential interactions with other nutrients, such as calcium and magnesium.
Rich Dietary Sources
- Animal-based: dairy products, meat, poultry, fish, and eggs provide highly bioavailable phosphorus in the form of organic phosphates.
- Plant-based: legumes, nuts, and whole grains contain phosphorus mainly as phytic acid; absorption can be lower but improved with proper preparation techniques.
- Food additives: many processed foods contain inorganic phosphate additives, which are absorbed more readily and can contribute significantly to total intake.
Recommended Intake and Balance
The recommended dietary allowance (RDA) for adults typically ranges between 700 and 1250 mg per day, depending on age, sex, and physiological status. A balanced calcium-to-phosphorus ratio (around 1:1 to 1.3:1) ensures optimal mineral deposition in bone. Excessive phosphorus intake, particularly from additives, may lead to disruption in calcium homeostasis, increasing the risk of bone demineralization.
Clinical Perspectives and Future Directions
Understanding the complexities of phosphorus metabolism offers insights into preventing and managing bone-related disorders. Clinicians must consider not only serum levels but also dietary habits, renal function, and hormonal status.
Diagnostic and Therapeutic Approaches
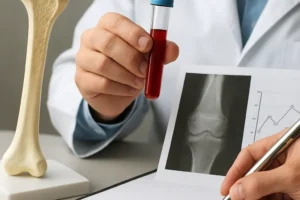
- Serum phosphorus measurements are standard in evaluating bone health and kidney function, yet they may not reflect total body stores accurately.
- Imaging techniques such as dual-energy X-ray absorptiometry (DXA) assess bone mineral density but cannot distinguish between calcium and phosphorus content.
- Therapeutic interventions range from dietary modification to phosphate binders in patients with chronic kidney disease, aiming to prevent vascular calcification and preserve skeletal integrity.
Emerging Research
Recent studies target molecular pathways that regulate phosphate transporters (e.g., NaPi-IIa, NaPi-IIc) and explore novel agents that modulate FGF23 or PTH activity. Regenerative medicine approaches are investigating how phosphorus-enriched scaffolds can enhance bone healing in orthopedic surgery. The interplay between the gut microbiome and phosphorus absorption also represents a promising avenue for optimizing nutrient utilization.
By deepening our knowledge of phosphorus dynamics, the medical community can develop more precise strategies to promote bone resilience, prevent age-related degeneration, and support patient-specific nutritional plans that foster lifelong skeletal health.