The intricate balance between bone strength and resilience extends beyond mere mass. While bone quantity—often measured by density—has traditionally dominated clinical assessments, emerging research highlights the pivotal role of bone quality in determining fracture risk and overall skeletal health. This article delves into the multifaceted aspects of bone biology, contrasts the methods for evaluating bone mass versus architectural integrity, and explores how these insights inform modern therapeutic strategies.
Importance of Bone Quality
Bone quality refers to the composite of characteristics that contribute to a bone’s ability to resist fracture. It encompasses factors such as microarchitecture, matrix composition, and the dynamic process of remodeling. While two individuals may exhibit similar bone mineral density (BMD), disparities in quality can lead to drastically different outcomes under mechanical stress.
Biological Composition of the Bone Matrix
- Collagen Framework: The organic scaffold of bone consists mainly of type I collagen, imparting tensile strength and flexibility.
- Hydroxyapatite Crystals: Mineral deposition within the collagen network provides compressive strength, augmented by optimal mineralization.
- Non-collagenous Proteins: Osteocalcin, osteonectin, and proteoglycans modulate crystal growth and interconnectivity.
Microarchitecture and Spatial Organization
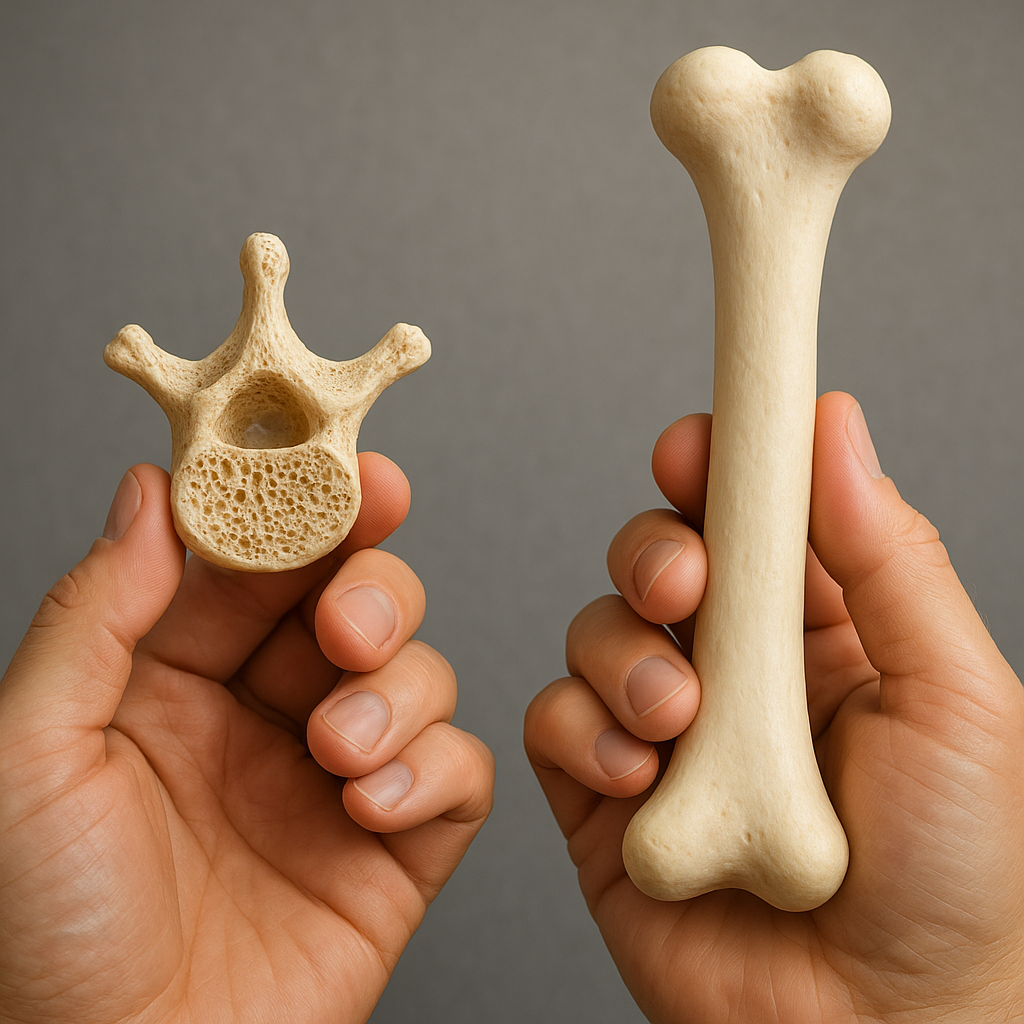
The internal arrangement of bone tissue divides into trabecular (spongy) and cortical (compact) compartments. Trabecular bone presents a lattice-like structure that dissipates loads, while cortical bone forms the dense outer shell. Disruptions in this arrangement—such as thinning of trabeculae or increased cortical porosity—can severely compromise strength despite preserved overall mass.
Key architectural parameters include:
- Trabecular thickness, number, and separation
- Cortical thickness and porosity
- Connectivity density of the trabecular network
Assessing Bone Quantity vs. Quality
Historically, clinicians have relied on bone mineral density as a surrogate marker for fracture risk. However, advanced imaging and biochemical markers now offer a richer portrait of skeletal integrity.
Bone Mineral Density and Dual-Energy X-ray Absorptiometry (DXA)
DXA remains the gold standard for diagnosing osteoporosis, measuring areal BMD in grams per square centimeter. While highly reproducible, it does not differentiate between trabecular and cortical compartments and provides limited insight into bone geometry or microarchitecture.
Quantitative Computed Tomography (QCT) and High-Resolution Techniques
- QCT: Offers volumetric BMD and separate evaluation of trabecular and cortical compartments, enabling a more detailed assessment of skeletal quality.
- High-Resolution Peripheral QCT (HR-pQCT): Captures microarchitectural indices at peripheral sites such as the wrist and tibia, quantifying parameters like trabecular thickness and cortical porosity with micrometer precision.
Biochemical Markers of Bone Turnover
Markers such as C-terminal telopeptide (CTX) and Procollagen Type I N-Terminal Propeptide (P1NP) reflect the rates of bone resorption and formation. Elevated CTX may indicate excessive osteoclastic activity, while P1NP levels correlate with osteoblastic synthesis. Integrating these markers with imaging can help discern whether low bone mass arises from slow formation, rapid resorption, or both.
Clinical Implications and Treatment Strategies
Understanding the interplay between quality and quantity transforms therapeutic decision-making. A patient with borderline BMD but severely compromised microarchitecture may benefit from interventions distinct from those prescribed to a patient with low mass but preserved quality.
Pharmacological Interventions
- Antiresorptives (e.g., bisphosphonates, denosumab): Primarily reduce bone resorption, increasing BMD and improving microstructure by filling cortical pores.
- Anabolics (e.g., teriparatide, abaloparatide): Stimulate osteoblastic activity, enhancing trabecular connectivity and increasing overall bone volume.
- Combination Therapy: Sequential or concomitant use of antiresorptives and anabolics can optimize both mass and quality, especially in high-risk individuals.
Lifestyle and Nutritional Considerations
Bone health depends on more than pharmaceuticals. Key modifiable factors include:
- Dietary calcium and vitamin D intake to support mineral deposition
- Regular weight-bearing and resistance biomechanics-based exercises to stimulate remodeling and increase bone density
- Avoidance of smoking and excessive alcohol consumption, both of which impair collagen cross-linking and bone turnover
Research Frontiers and Future Directions
Cutting-edge studies are exploring the genetic and molecular determinants of bone quality, aiming to uncover novel targets for therapy. Gene editing and stem cell approaches hold promise for correcting intrinsic deficiencies in matrix proteins or cellular signaling pathways. Moreover, advances in imaging—such as ultra-high-field magnetic resonance and photon-counting computed tomography—may soon enable comprehensive in vivo characterization of bone at the nanoscale.
Biomechanical Modeling and Predictive Analytics
Finite element analysis integrates imaging data to simulate stress distribution and predict fracture risk under various loading scenarios. These models can personalize risk assessment, guiding clinicians in tailoring both pharmacological regimens and lifestyle recommendations.
Biomaterials and Bone Tissue Engineering
Developments in scaffold design and growth factor delivery offer potential for regenerating bone with optimized microarchitecture. Biodegradable composites laden with osteoinductive peptides aim to encourage seamless integration with native bone, enhancing both volume and quality.
Conclusion
Evaluating bone health requires a dual focus on mass and material characteristics. While BMD provides a convenient benchmark, comprehensive skeletal assessment—encompassing microarchitecture, turnover markers, and biomechanical competence—yields a richer understanding of fracture risk. As research continues to unravel the molecular underpinnings of bone quality, clinical practice must adapt, embracing multifaceted strategies to reinforce the skeleton from the inside out.