Maintaining a robust skeletal system is fundamental to overall health, yet the decline in daily activity levels has introduced significant challenges to bone integrity. Exploring the multifaceted impact of physical inactivity on the skeleton reveals complex interactions among cellular processes, hormonal balances, and mechanical forces. This article examines the underlying mechanisms, epidemiological trends, clinical consequences, and potential interventions aimed at preserving or restoring bone strength in sedentary populations.
Cellular and Molecular Mechanisms of Bone Loss
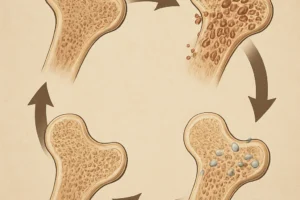
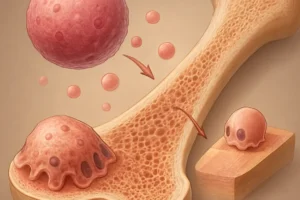
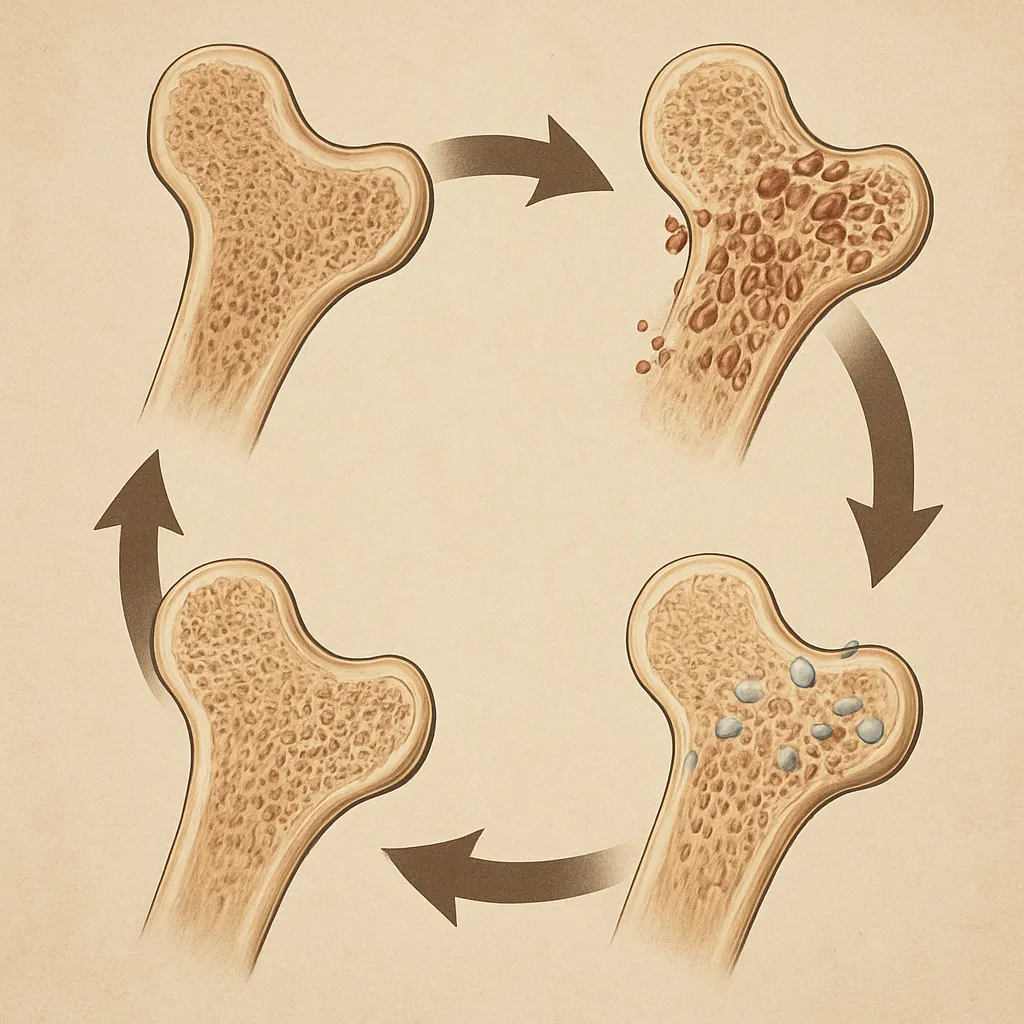
Bone is a dynamic tissue undergoing continuous remodeling through the coupled activities of osteoblasts (bone-forming cells) and osteoclasts (bone-resorbing cells). Mechanical stimuli drive adaptation via the mechanostat model, which posits that bones sense strain and adjust mass to maintain optimal strength. Inactivity disrupts this equilibrium.
Reduced Mechanical Loading
Under sedentary conditions, reduced ground reaction forces and muscle contractions translate to diminished osteogenic signals. The lack of compressive and tensile strain leads to:
- Downregulation of bone anabolic pathways, including Wnt/β-catenin signaling
- Decreased expression of growth factors such as IGF-1 and TGF-β
- Altered osteocyte function, with fewer lacunar signals to orchestrate remodeling
Cellular Imbalance
When mechanical cues wane, osteoclast activity may exceed osteoblast function, resulting in net bone loss. Key features include:
- Elevated RANKL/OPG ratio, favoring resorption
- Reduced osteoblast proliferation and differentiation
- Impaired mitochondrial function in bone cells, leading to energy deficits
Hormonal and Metabolic Influences
Physical inactivity also impacts endocrine regulators:
- Lowered circulating levels of estrogen and testosterone, exacerbating bone turnover
- Insulin resistance and chronic inflammation, both of which can stimulate osteoclastogenesis
- Alterations in parathyroid hormone rhythm, potentially increasing calcium mobilization
Risk Factors and Epidemiological Trends
Global trends indicate an increasing prevalence of sedentary lifestyles, driven by urbanization, technology use, and occupational shifts. This epidemiological shift correlates with a rise in bone fragility conditions.
Demographic Vulnerabilities
- Older adults experience sarcopenia and inactivity, compounding bone loss
- Postmenopausal women face estrogen deficiency, heightening osteoporosis risk
- Adolescents with sedentary habits may fail to achieve peak bone density
Lifestyle and Comorbidities
- Obesity generates inflammatory cytokines and fosters insulin resistance
- Smoking and alcohol consumption synergize with inactivity to accelerate skeletal degradation
- Chronic diseases like diabetes and rheumatoid arthritis often correlate with reduced mobility
Regional and Socioeconomic Disparities
- Urban populations may have fewer opportunities for weight-bearing exercise
- Lower socioeconomic status often limits access to recreational facilities and healthy diets
- Cultural norms influence gender-specific activity levels, impacting bone health differentially
Clinical Implications and Fracture Risk
Impaired skeletal strength from inactivity manifests as increased fracture risk, higher morbidity, and greater healthcare burdens. Recognizing early signs and quantifying risk are essential to preventing adverse outcomes.
Diagnostic Assessment
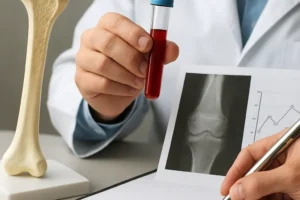
Key modalities include:
- Dual-energy X-ray absorptiometry (DXA) to measure areal bone mineral density
- Quantitative ultrasound and peripheral CT scans for microarchitectural evaluation
- Biochemical markers of bone turnover, such as serum CTX and P1NP
Clinical Presentations
- Vertebral compression fractures leading to kyphosis and chronic back pain
- Hip fractures, frequently requiring surgical intervention and prolonged rehabilitation
- Fragility fractures of the wrist and humerus, often heralding generalized skeletal weakness
Economic and Quality-of-Life Impact
- Extended hospital stays and increased likelihood of institutional care post-fracture
- Loss of independence, psychological distress, and diminished physical function
- Substantial healthcare costs related to acute treatment and long-term management
Prevention and Therapeutic Strategies
Combating the consequences of inactivity necessitates a multifaceted approach, integrating exercise, nutritional optimization, pharmacology, and behavioral interventions.
Exercise and Mechanical Loading
- Weight-bearing aerobic activities (e.g., brisk walking, jogging) to stimulate bone formation
- Resistance training targeting major muscle groups, enhancing bone–muscle interactions
- High-impact exercises (e.g., jumping, plyometrics) for young adults to maximize peak mass
Nutritional and Lifestyle Modifications
- Ensuring adequate calcium and vitamin D intake to support mineralization
- Protein-rich diets for collagen synthesis and muscle maintenance
- Avoidance of tobacco and moderation of alcohol to reduce catabolic effects
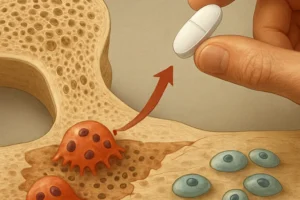
Pharmacological Interventions
- Antiresorptives (bisphosphonates, denosumab) to inhibit osteoclast-mediated bone loss
- Anabolics (teriparatide, abaloparatide) to promote osteoblast-driven formation
- Selective estrogen receptor modulators and hormone replacement in appropriate patients
Rehabilitation and Behavioral Support
Structured rehabilitation programs and behavioral counseling play a vital role:
- Physiotherapy to restore mobility and prevent deconditioning
- Motivational interviewing and digital health tools to encourage adherence
- Community-based initiatives fostering social engagement and active lifestyles