The relationship between dietary protein and skeletal health has gained significant attention within the fields of bone biology and nutrition. Adequate protein intake plays a crucial role in maintaining density and structural integrity, influencing processes such as collagen formation, calcium absorption, and overall bone turnover. Emerging research suggests that both the quantity and quality of protein consumed can modulate fracture risk and the progression of conditions like osteoporosis. This article explores the underlying mechanisms of protein’s action on the skeleton, evaluates dietary recommendations, and examines clinical implications for maximizing bone strength through nutrition.
Protein Metabolism and Bone Remodeling
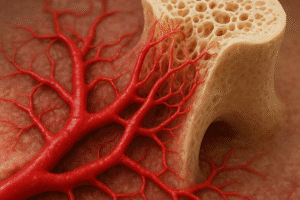
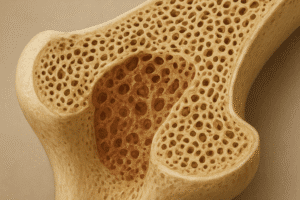
Bone is a dynamic tissue undergoing continuous cycles of resorption and formation in a process known as remodeling. Osteoclasts degrade old bone matrix while osteoblasts synthesize new bone, depositing collagen and mineralizing the matrix with calcium and phosphate. Amino acids derived from dietary protein are vital substrates for osteoblasts, contributing to the synthesis of collagen type I, the predominant organic component of bone.
The interplay between protein consumption and bone metabolism involves several key pathways:
- Amino Acids Supply: Essential amino acids such as lysine, proline, and glycine are incorporated into collagen fibrils, establishing tensile strength and resilience.
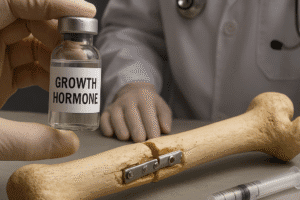
- Growth Factors Modulation: Insulin-like growth factor 1 (IGF-1) is synthesized in response to adequate protein intake, stimulating osteoblast proliferation and differentiation.
- Hormonal Regulation: Dietary protein affects levels of parathyroid hormone (PTH), which directly influences osteoclastic activity and calcium homeostasis.
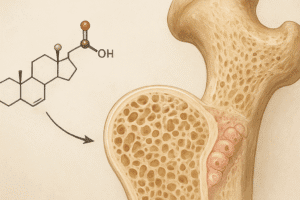
- Acid-Base Balance: Sulfur-containing amino acids can generate an acid load; however, this effect is often counterbalanced by alkaline food components such as fruits and vegetables. Net balance influences bone resorption rates.
These mechanisms illustrate why insufficient protein leads to reduced bone formation, compromised matrix quality, and increased fracture susceptibility, whereas optimal protein status supports robust bone architecture.
Dietary Protein Sources and Recommendations
A variety of proteins contribute to skeletal health, categorized broadly into animal and plant sources. Animal proteins from dairy, meat, poultry, and fish provide high bioavailability of all essential amino acids. Plant-based proteins—found in legumes, nuts, seeds, and whole grains—often lack one or more amino acids but can be combined to meet requirements.
Key considerations for selecting protein sources include digestibility, amino acid profile, and associated nutrients:
- Dairy Products: Milk, yogurt, and cheese supply both calcium and protein, exerting a synergistic effect on bone mineralization.
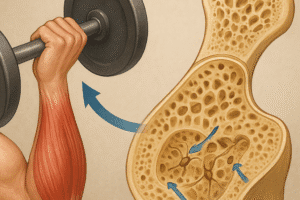
- Lean Meats and Poultry: High-quality proteins with minimal saturated fat content support muscle mass preservation, which indirectly benefits bone integrity through mechanical loading.
- Fish and Seafood: Rich in omega-3 fatty acids, consumption may reduce inflammation and promote bone formation.
- Legumes and Soy: Offer phytoestrogens that may mimic estrogenic effects on bone, particularly beneficial post-menopause.
- Mixed Plant Proteins: Combining grains and legumes (e.g., rice and beans) ensures a complete amino acid profile akin to animal proteins.
National and international guidelines recommend 0.8–1.2 g of protein per kilogram of body weight daily for healthy adults, with higher intakes (1.2–1.5 g/kg) advised for older individuals to offset sarcopenia and preserve bone density. Athletes and individuals recovering from injury may require up to 1.6 g/kg to support healing and remodeling processes.
Impact on Calcium Absorption and Bone Health
When evaluating protein’s effect on bone, the influence on calcium balance is often scrutinized. Early studies hypothesized that high protein diets induce hypercalciuria, leading to bone demineralization. However, contemporary research indicates that increased urinary calcium reflects greater intestinal absorption rather than net calcium loss from the skeleton.
Mechanisms by which protein enhances calcium homeostasis include:
- Intestinal Calcium Uptake: Amino acids such as arginine and lysine stimulate calcium transporters in the gut lining, improving fractional absorption.
- Hormonal Interactions: Elevated IGF-1 levels associated with protein intake may upregulate intestinal calcium-binding proteins, augmenting uptake.
- Buffering Effect: Dietary protein increases acid load; the kidney excretes excess acid along with calcium, but concurrent elevation in absorption compensates for urinary losses.
Clinical trials have demonstrated that diets balanced in protein and alkalizing nutrients (e.g., potassium-rich fruits) maintain neutral or positive calcium balance, thereby supporting bone mass accrual and reducing fracture risk, especially in the elderly.
Clinical Implications and Future Directions
Understanding the role of protein in metabolism and skeletal health has significant clinical applications. Nutritional strategies can be tailored to populations at risk of low bone mass, including:
- Postmenopausal Women: Combined protein and calcium interventions enhance bone mineral density (BMD) and reduce vertebral fractures.
- Older Adults: Protein supplementation may counteract age-related muscle loss, improving mobility and reducing fall-related fractures.
- Patients with Chronic Conditions: Individuals with renal disease require careful protein modulation to preserve kidney function without compromising bone strength.
Emerging research delves into the impact of specific amino acids and peptides on remodeling pathways, with studies investigating collagen hydrolysates, leucine-enriched blends, and bioactive peptides derived from dairy. These novel interventions aim to optimize synthesis of bone matrix components and modulate osteoblastic gene expression.
Future directions include large-scale randomized controlled trials to determine the optimal protein-to-calcium ratio, exploration of personalized nutrition based on genetic predisposition to bone disorders, and development of functional foods targeting skeletal health. By integrating precision nutrition with conventional therapies, clinicians may better prevent and manage osteoporosis and related fractures across the lifespan.