Bone disorders associated with genetic syndromes present complex challenges for clinicians and researchers alike. These conditions often arise from mutations affecting the development, structure, or remodeling of the skeleton. Understanding the underlying mechanisms and clinical features of these syndromes is essential for accurate diagnosis, effective management, and exploration of innovative therapies. This article explores key genetic bone disorders, diagnostic strategies, and emerging treatment modalities.
Overview of Genetic Bone Disorders
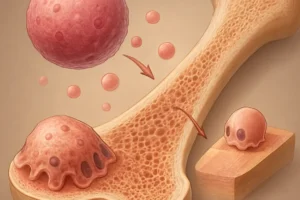
Genetic bone disorders encompass a diverse group of conditions in which alterations in DNA compromise the normal function of osteoblasts and osteoclasts, disrupt connective tissue integrity, or impair growth plate dynamics. Many of these syndromes are inherited in an autosomal dominant or recessive pattern, though sporadic mutations can also occur. Common hallmarks include reduced bone density, skeletal deformities, and an increased risk of fractures.
Key mechanisms underlying these disorders involve defects in:
- collagen synthesis and structure
- Growth factor receptor signaling in chondrocytes
- Extracellular matrix proteins such as fibrillin
- Bone mineralization pathways
By identifying the molecular roots of skeletal fragility, researchers aim to tailor interventions that target specific pathways rather than employing nonspecific supportive care alone.
Major Syndromes Affecting Bone Integrity
Osteogenesis Imperfecta
Osteogenesis Imperfecta (OI), commonly known as brittle bone disease, is most frequently linked to mutations in the COL1A1 or COL1A2 genes, which code for type I collagen. These defects produce structurally abnormal collagen fibrils, undermining bone strength and leading to recurrent fractures, blue sclerae, dentinogenesis imperfecta, and hearing loss. OI is categorized into several types ranging from mild to perinatally lethal:
- Type I: Mild, with few fractures and near-normal stature
- Type II: Lethal in utero or shortly after birth
- Type III: Severe, progressive deformities, short stature
- Type IV: Moderate, variable deformities
Management strategies focus on fracture prevention, pain control, and maximizing mobility. Intravenous bisphosphonates have become a mainstay to increase bone mass and reduce fracture incidence. Surgical interventions such as rodding procedures reinforce long bones, while physical therapy encourages safe weight-bearing activities. Ongoing research into gene therapy and cell-based treatments offers hope for more definitive cures.
Achondroplasia
As the most common cause of disproportionate short stature, Achondroplasia arises from gain-of-function mutations in the FGFR3 gene. This receptor normally inhibits chondrocyte proliferation in growth plates; the mutation amplifies its activity, prematurely arresting longitudinal bone growth. Clinically, affected individuals display a normal trunk, shortened limbs, macrocephaly, and characteristic facial features.
Complications include spinal stenosis, ear infections, and foramen magnum compression. Radiographic evaluation reveals flared metaphyses, narrowed interpedicular distances, and trident hands. Management is multidisciplinary, involving neurosurgical decompression when necessary, growth hormone therapy in select cases, and physical support to optimize motor development.
Marfan Syndrome
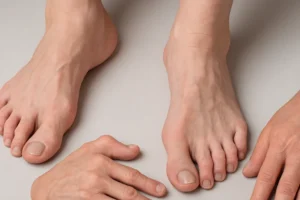
In Marfan Syndrome, mutations in the FBN1 gene disrupt fibrillin-1, a glycoprotein vital for elastic fiber formation in connective tissues. While cardiovascular and ocular manifestations often dominate, skeletal involvement includes long limbs, pectus excavatum or carinatum, scoliosis, and joint laxity. The phenotype reflects overgrowth of long bones and ligamentous laxity.
Diagnosis relies on Ghent nosology criteria, integrating family history, physical signs, and molecular testing. Regular monitoring of aortic root dimensions via radiography and echocardiography guides prophylactic beta-blocker use or surgical repair. Exercise modification and targeted physiotherapy help maintain musculoskeletal health.
Ehlers-Danlos Syndrome
Ehlers-Danlos Syndrome (EDS) comprises a heterogeneous group of connective tissue disorders affecting skin, joints, and vasculature. Several subtypes stem from mutations in genes encoding various collagens or enzymes involved in collagen processing. Classical EDS features skin hyperextensibility and joint hypermobility, while vascular EDS can lead to life-threatening arterial ruptures.
Skeletal manifestations include frequent joint dislocations, pes planus, and early-onset osteoarthritis. Management prioritizes joint stabilization, activity modification, and pain control. Customized orthotics and targeted strengthening exercises enhance proprioception and reduce injury risk.
Diagnostic Approaches and Imaging
Early recognition of genetic bone disorders is crucial for preventing complications and improving long-term outcomes. A comprehensive evaluation typically involves:
- Detailed family and medical history
- Physical examination focusing on limb proportions, joint range of motion, and skin findings
- Laboratory assays for bone turnover markers
- Advanced imaging studies
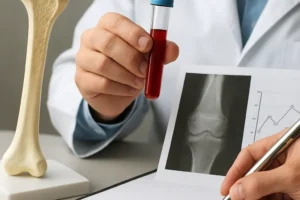
radiography remains the cornerstone for assessing bone morphology, fracture patterns, and deformities. Dual-energy X-ray absorptiometry (DEXA) quantifies bone density to track osteoporosis or osteopenia. Magnetic resonance imaging (MRI) and computed tomography (CT) can evaluate spinal canal dimensions, detect subtle fractures, and assess soft tissue integrity around joints.
Genetic testing, including targeted gene panels or whole-exome sequencing, confirms specific mutations and facilitates family counseling. Prenatal diagnostics, such as chorionic villus sampling or amniocentesis, may be offered to families with known high-risk alleles.
Therapeutic Strategies and Future Directions
Interventions for genetic bone disorders span pharmacologic, surgical, and rehabilitative modalities. Key approaches include:
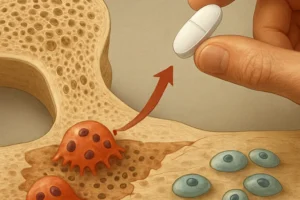
- Anti-resorptive agents (e.g., bisphosphonates, denosumab) to reduce fracture rates
- Anabolic therapies (e.g., teriparatide) to stimulate osteoblast activity
- Orthopedic surgeries for deformity correction and stabilization
- Physiotherapy to enhance muscle strength and joint stability
Emerging treatments target molecular pathways directly. Small-molecule inhibitors of mutant FGFR3 show promise for Achondroplasia, while antisense oligonucleotides may correct aberrant splicing in certain forms of OI. Advances in stem cell biology are fueling research into mesenchymal stem cell transplantation to repopulate defective bone tissue. Moreover, CRISPR/Cas9 genome editing might one day enable precise correction of pathogenic variants.
Collaboration among geneticists, orthopedic surgeons, endocrinologists, and physical therapists is vital to deliver personalized care. As our understanding of skeletal biology deepens, the integration of novel diagnostics and targeted therapies holds the potential to transform the prognosis for individuals with genetic bone disorders.