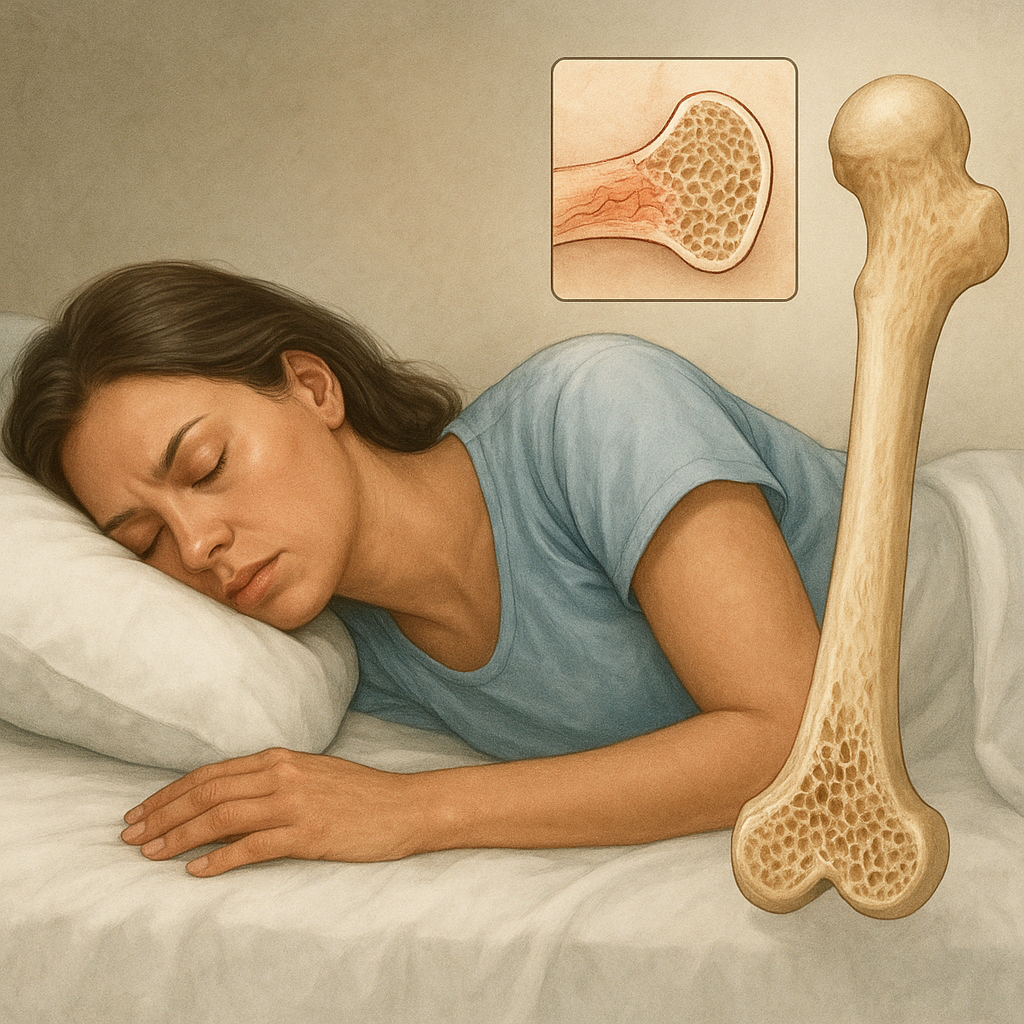
Sleep quality extends its influence far beyond cognitive function and mood regulation. Recent research underscores the significant impact of disordered sleep on skeletal integrity. Understanding the interplay between nocturnal rest and bone metabolism is essential for clinicians, patients, and researchers aiming to prevent long-term musculoskeletal complications.
Biological Mechanisms Linking Sleep and Bone Health
Hormonal Regulation and Circadian Rhythms
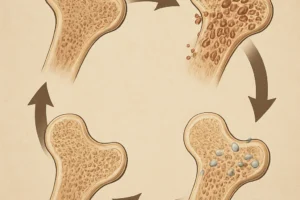
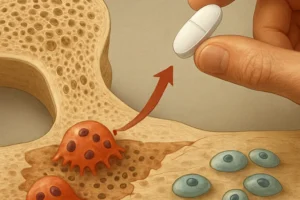
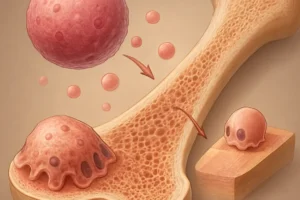
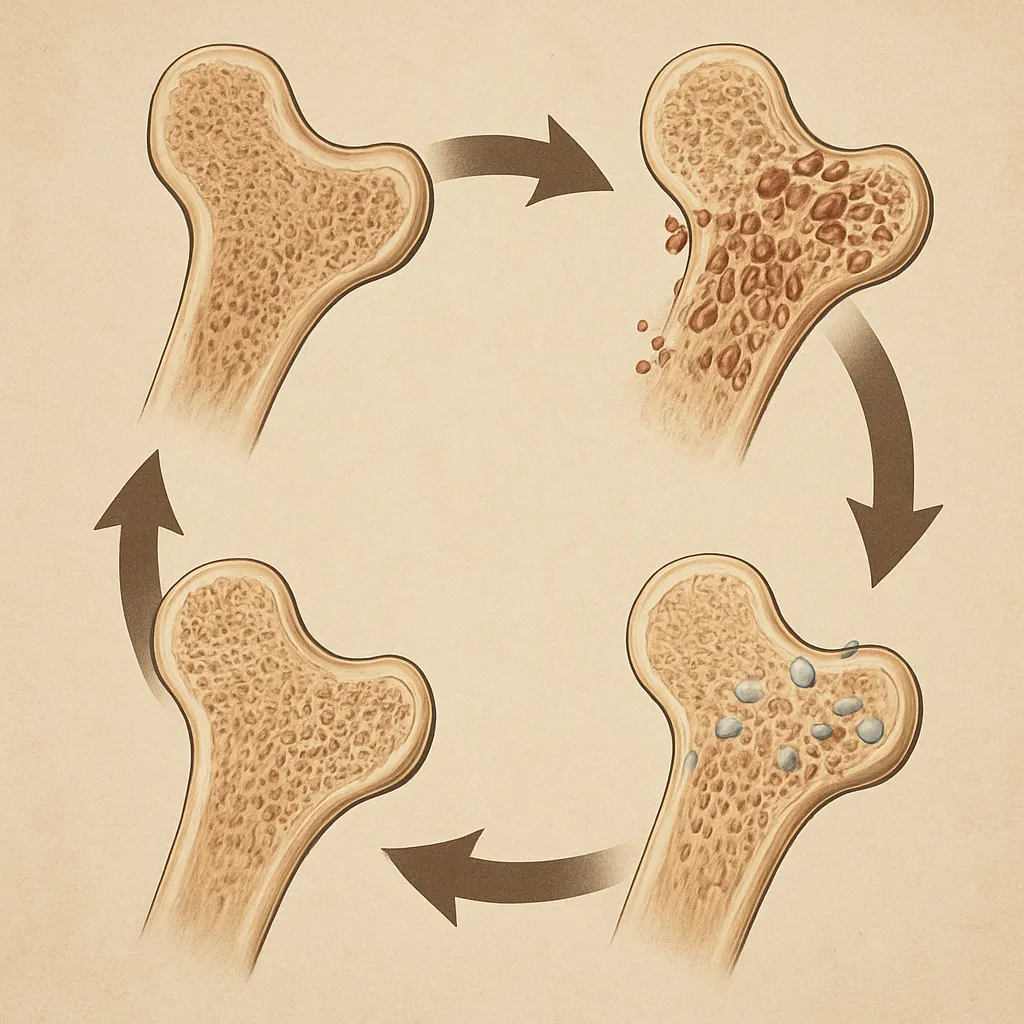
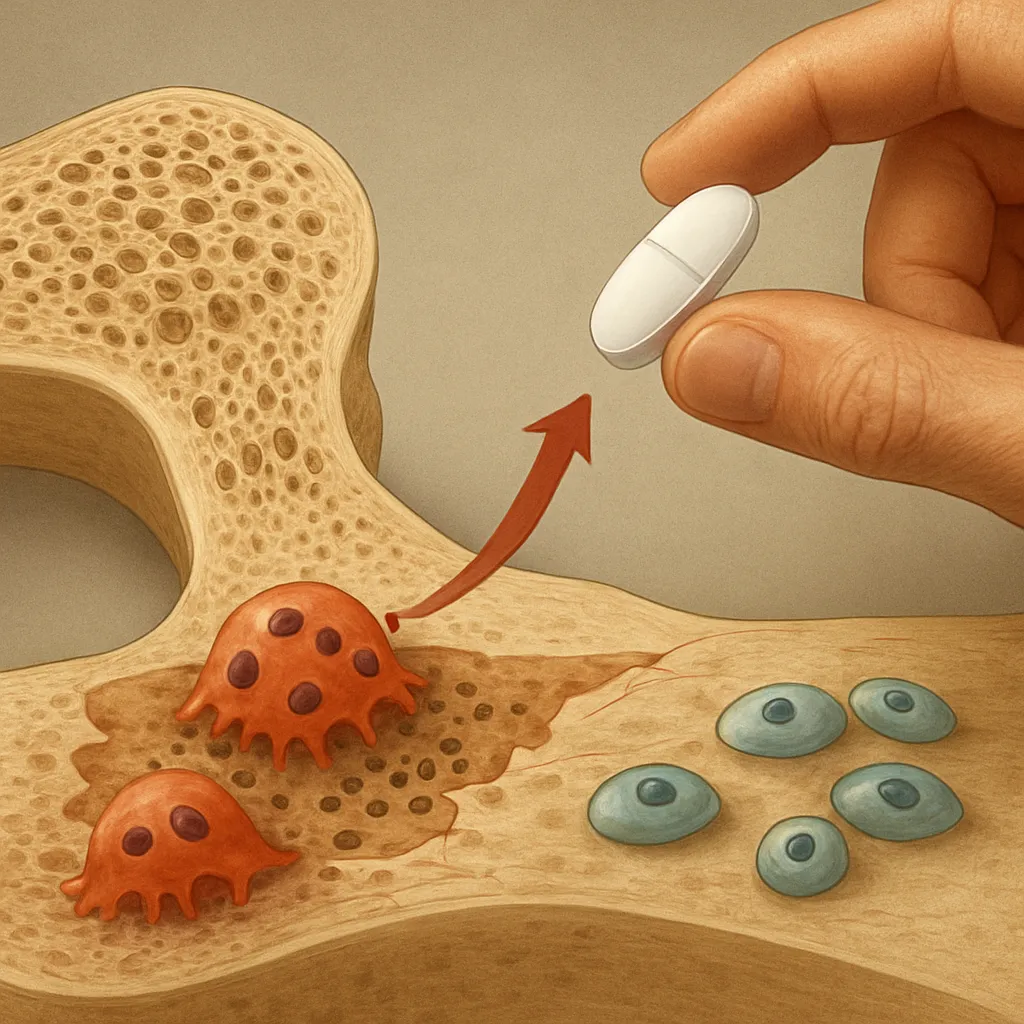
The skeleton is not a static structure; it undergoes continuous bone remodeling through coordinated activity of osteoblasts and osteoclasts. This process is tightly regulated by the endocrine system and follows a circadian pattern. Disruption of the circadian rhythm can impair the release of key hormones:
- Melatonin: Secreted during darkness, melatonin promotes osteoblast differentiation and suppresses osteoclast activity. Reduced melatonin levels are linked to lower bone density.
- Growth Hormone (GH): Peaks during slow-wave sleep, essential for cartilage formation and bone growth.
- Parathyroid Hormone (PTH): Exhibits diurnal variation; sleep deprivation can alter PTH secretion, leading to calcium imbalance.
Inflammatory Pathways
Chronic sleep loss or fragmentation triggers a pro-inflammatory state characterized by elevated cytokines such as interleukin-6 and tumor necrosis factor-alpha. This systemic inflammation accelerates bone resorption and impairs matrix synthesis.
Metabolic Factors
Insufficient sleep often correlates with insulin resistance and altered lipid metabolism. Both conditions can adversely affect bone by:
- Reducing osteoblast proliferation.
- Increasing advanced glycation end-products (AGEs) in bone collagen, making the matrix more brittle.
Common Sleep Disorders and Bone Consequences
Obstructive Sleep Apnea (OSA)
Characterized by recurrent airway collapse and intermittent hypoxia, OSA unleashes oxidative stress and inflammatory mediators that compromise bone microarchitecture. Studies indicate a correlation between OSA severity and reduced bone density, increasing the risk of stress fractures.
Insomnia and Sleep Fragmentation
Chronic insomnia leads to fragmented sleep patterns that blunt nocturnal hormone pulses. Patients with long-term insomnia exhibit lower levels of GH and melatonin, risking reduced mineralization and osteopenia.
Restless Legs Syndrome (RLS) and Periodic Limb Movement Disorder (PLMD)
RLS and PLMD often result in micro-awakenings, depriving individuals of restorative phases of sleep. As a consequence, bone turnover markers suggest heightened resorption without proportional formation.
Clinical Evidence and Epidemiological Studies
Cross-Sectional Observations
Population surveys have documented associations between self-reported sleep duration and bone mineral density (BMD). Individuals sleeping less than six hours nightly show significantly lower hip and lumbar BMD compared to those with seven to eight hours of sleep.
Longitudinal Cohorts
Prospective cohorts tracking middle-aged adults over a decade reveal that persistent sleep disturbances predict greater bone loss and higher incidence of fragility fractures. Adjusted for confounders like age, body mass index, smoking, and physical activity, sleep quality remains an independent risk factor.
Interventional Trials
Clinical trials investigating Continuous Positive Airway Pressure (CPAP) therapy in OSA patients report modest improvements in markers of bone formation after six months of consistent use. However, long-term benefits on actual BMD require further investigation.
Strategies to Protect Bone Health in Sleep-Disordered Patients
Optimizing Sleep Hygiene
Fundamental interventions include:
- Maintaining a regular sleep–wake schedule.
- Limiting exposure to screens before bedtime.
- Ensuring a dark, cool, and quiet sleep environment.
These measures support normalization of the circadian rhythm, enhancing nocturnal hormone release vital for bone health.
Medical Management of Sleep Disorders
Specific treatments tailored to the disorder can mitigate bone risk:
- Obstructive Sleep Apnea: CPAP therapy reduces intermittent hypoxia and systemic inflammation.
- Insomnia: Cognitive-behavioral therapy for insomnia (CBT-I) restores sleep architecture and improves GH and melatonin secretion.
- RLS/PLMD: Dopaminergic agents or iron supplementation may decrease limb movements, preserving restorative sleep stages.
Nutritional and Lifestyle Considerations
Optimal bone health demands a comprehensive approach:
- Nutrition: Adequate calcium and vitamin D intake supports mineralization. Nutrients such as magnesium and vitamin K2 also play roles in bone matrix quality.
- Exercise: Weight-bearing and resistance training stimulate osteoblast activity and enhance bone density.
- Smoking Cessation and Alcohol Moderation: Both factors negatively affect hormone balance and fracture risk.
Integrating Sleep and Bone Health in Clinical Practice
Healthcare providers should incorporate sleep assessments into routine osteoporosis risk evaluations. Simple screening tools, actigraphy, or polysomnography may identify patients at elevated risk. Early intervention targeting both sleep quality and skeletal care can offer synergistic benefits.
Future Directions
Further research should elucidate mechanistic pathways linking distinct sleep stages with specific phases of bone remodeling. Large-scale randomized trials are necessary to confirm whether sleep-focused therapies can significantly reduce fracture incidence in high-risk populations.