The prolonged use of various pharmacological agents can profoundly influence skeletal integrity, necessitating a careful evaluation of risks and benefits in clinical practice. As more patients rely on medications for chronic conditions, understanding how these drugs interact with bone tissue is essential. This article explores the multifaceted relationship between long-term medication use and skeletal health, examining common culprits, underlying mechanisms, and practical strategies to mitigate adverse effects.
Common Medications and Their Impact on Bone
Several drug classes have been consistently associated with compromised bone strength and increased fracture risk. Clinicians must remain vigilant when prescribing these agents for extended periods.
- Glucocorticoids: Widely used for autoimmune disorders and chronic inflammatory diseases, these steroids accelerate bone resorption and inhibit formation, often leading to significant osteoporosis within months of initiation.
- Antiepileptic drugs (e.g., phenytoin, carbamazepine): These medications alter vitamin metabolism and reduce bone density, raising the likelihood of stress fractures.
- Proton pump inhibitors (PPIs): Chronic acid suppression interferes with intestinal absorption of calcium and vitamin D, contributing to suboptimal mineralization and elevated fracture incidence.
- Thyroid hormone replacement in excess: Over-treatment can induce a hypermetabolic state that speeds up bone remodeling and causes net bone loss.
- Aromatase inhibitors: Employed in hormone-sensitive breast cancer, they diminish estrogen levels, undermining the protective effect of estrogen on the female skeleton.
While these agents offer clear therapeutic advantages, awareness of their skeletal side effects allows for early intervention. A multidisciplinary approach—engaging endocrinologists, pharmacists, and primary care providers—yields the best outcomes for bone preservation.
Mechanisms Underlying Medication-Induced Bone Loss
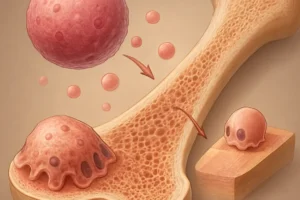
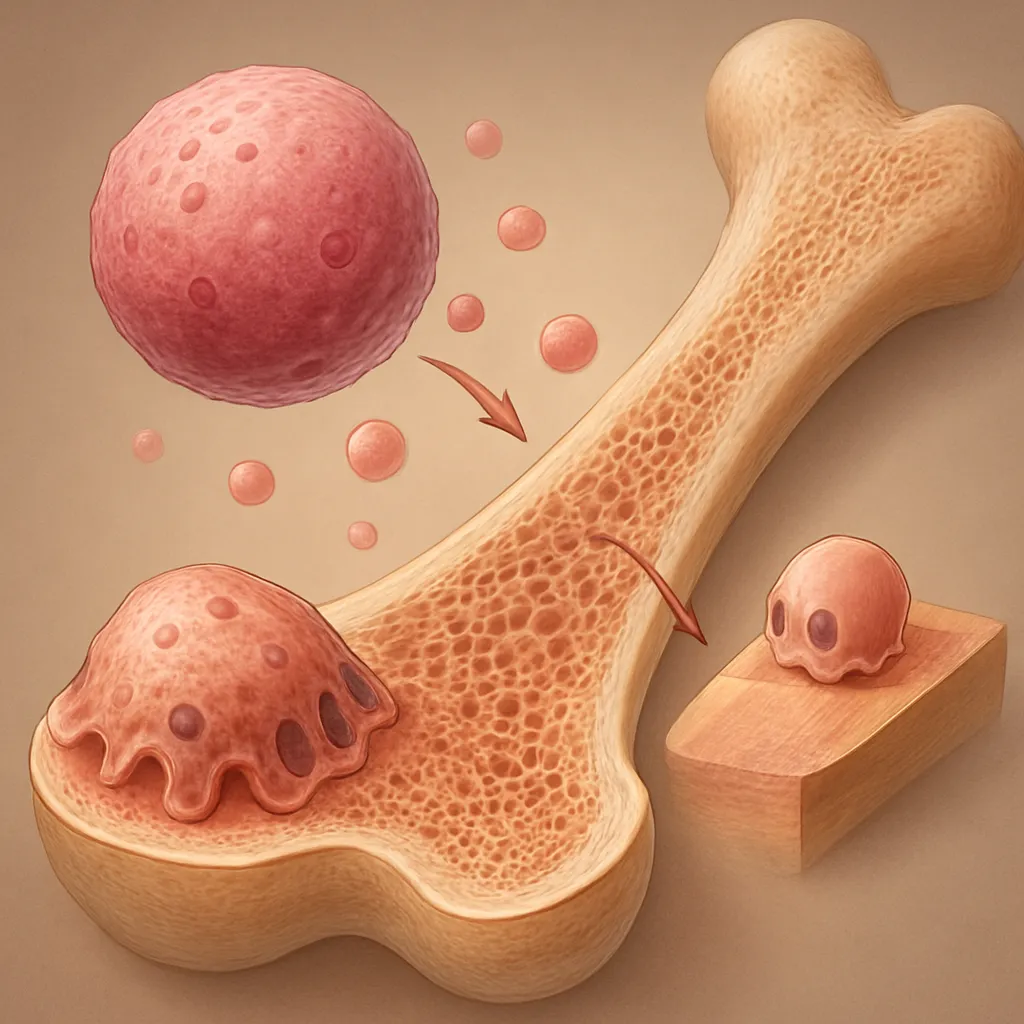
Bone health depends on a delicate equilibrium between osteoclast-mediated resorption and osteoblast-driven formation. Disruption of this balance by medications can occur through several pathways:
Hormonal Modulation
Drugs that mimic or obstruct endogenous hormones substantially affect bone cells. For example, glucocorticoids reduce gonadotropin release, leading to secondary hypogonadism and diminished sex steroid support of bone. Similarly, aromatase inhibitors lower estrogen, a hormone vital for suppressing osteoclast activity.
Direct Cellular Effects
Certain agents exert cytotoxic effects on osteoblasts and osteocytes, the architects of bone matrix. Long-term corticosteroid exposure induces apoptosis of these cells, impairing new bone synthesis. Conversely, some anti-cancer chemotherapies trigger oxidative stress and DNA damage, leading to compromised bone cell viability.
Altered Mineral Homeostasis
Gastrointestinal and renal effects of medications can derail electrolyte balance. PPIs, through reduced gastric acidity, limit absorption of calcium, while loop diuretics increase urinary calcium excretion. Imbalances in phosphate and magnesium may further disturb mineral deposition within the matrix.
Inflammatory and Immune Pathways
Drugs intended to quell inflammation can paradoxically disrupt bone remodeling. TNF-alpha inhibitors, though generally protective by dampening cytokine-mediated bone loss, occasionally trigger shifts in immune cell populations that indirectly influence osteoclast differentiation.
Strategies for Prevention and Support of Bone Health
Early recognition of at-risk individuals and implementation of prophylactic measures are paramount. The following approaches are recommended:
- Baseline assessment of bone density via dual-energy X-ray absorptiometry (DXA) before initiating high-risk therapies.
- Supplementation with calcium and vitamin D to offset malabsorption and promote mineralization.
- Consideration of anti-resorptive agents, such as bisphosphonates or denosumab, for patients on chronic glucocorticoid therapy.
- Utilization of anabolic therapies (e.g., teriparatide) in severe cases to stimulate bone formation.
- Regular physical activity emphasizing weight-bearing exercises to enhance mechanical loading and bone strength.
- Monitoring of serum markers and imaging studies at 6–12 month intervals to gauge response and adjust treatment.
Patient education on lifestyle factors—such as smoking cessation, alcohol moderation, and fall prevention—is equally crucial. Encouraging dietary modifications that include leafy greens and dairy products supports overall skeletal resilience.
Emerging Therapies and Research Directions
Ongoing research seeks novel agents that selectively target bone cells with minimal systemic side effects. Key areas of innovation include:
Sclerostin Inhibitors
Monoclonal antibodies against sclerostin remove an inhibitory signal on osteoblasts, promoting robust bone formation without substantially affecting resorption. Early trials demonstrate significant increases in vertebral and hip bone mineral density.
RANK Ligand Modulation
Beyond denosumab, small molecule inhibitors of RANK ligand signaling are under investigation. These compounds aim to fine-tune osteoclast activity and reduce the risk of oversuppression that can lead to atypical fractures.
Microbiome-Based Interventions
Gut microbiota influence nutrient absorption and immune regulation. Probiotics and prebiotics designed to enrich beneficial bacterial populations may indirectly bolster bone health, particularly in patients with PPI-induced dysbiosis.
Personalized Medicine Approaches
Genetic profiling and biomarker analysis promise to identify individuals predisposed to medication-induced bone loss. Tailored regimens—adjusting drug type, dose, and duration—could minimize skeletal side effects while preserving therapeutic efficacy.
Collaboration between pharmaceutical developers and clinical researchers remains vital to accelerate the translation of these innovations into practice. Enhanced monitoring protocols and improved patient adherence tools, such as digital health applications, will further optimize long-term outcomes for those requiring chronic medication.