Chronic infections pose a significant threat to bone health by disrupting the dynamic balance of bone remodeling. This article examines how persistent pathogens impact bone integrity, explores the underlying molecular pathways, highlights specific microbial culprits, and reviews diagnostic and treatment options within the field of bone and medicine.
Chronic Infections and Systemic Inflammation
Persistent microbial challenges trigger a sustained inflammation state that adversely affects skeletal health. Immune cells release cytokines which modulate bone remodeling by activating osteoclasts and inhibiting osteoblast function. The result is an imbalance favoring bone resorption, undermining overall bone strength. Systemic effects extend beyond local lesions, linking chronic diseases such as rheumatoid arthritis and periodontitis with reduced mineral density. Chronic inflammatory states associated with bone pathology often resemble features of osteoporosis, characterized by decreased bone mass and microarchitectural deterioration. Emerging data suggests that the gut microbiome also plays a crucial role by shaping immune responses and metabolite profiles that influence remote bone sites.
Mechanisms of Bone Destruction
At the cellular level, infections can hijack normal bone remodeling processes through several overlapping pathways. Bacterial toxins and viral proteins stimulate RANKL expression, a key driver of osteoclastogenesis. As activated osteoclasts increase in number, the resorptive surface expands, accelerating bone loss. Meanwhile, inflammatory mediators such as tumor necrosis factor alpha and interleukin 1 disrupt osteoblast differentiation and survival. The net effect is compromised matrix deposition and mineralization. In addition, certain pathogens produce enzymes that degrade collagen and other extracellular matrix components, directly eroding the structural framework of bone. Hypoxia induced by chronic infection further impairs osteoblast activity, compounding the risk of microarchitectural collapse. Understanding these mechanisms is essential for developing targeted interventions to preserve bone integrity.
Specific Pathogens and Bone Disease
Certain microorganisms exhibit tropism for skeletal tissues, leading to characteristic bone pathologies:
- Mycobacterium tuberculosis: causes spinal tuberculosis (Pott disease), leading to vertebral collapse and kyphotic deformity.
- Staphylococcus aureus: frequently responsible for acute and chronic osteomyelitis; biofilm formation on implants complicates eradication.
- Treponema pallidum: tertiary syphilis manifests as gummatous lesions in bone, resulting in progressive destruction.
- Borrelia burgdorferi: associated with Lyme arthritis, which can extend to subchondral bone erosion in chronic cases.
- Fungal species (e.g., Candida, Aspergillus): opportunistic infections in immunocompromised patients cause osteolytic lesions.
These agents share the ability to evade immune clearance, secrete destructive enzymes, and induce prolonged inflammation. In carriers of implantable devices, biofilm-mediated resistance often necessitates device removal and prolonged high-dose antibiotic therapy.
Diagnostic Approaches
Timely and accurate diagnosis of infection-related bone compromise is crucial to prevent irreversible damage. Key modalities include:
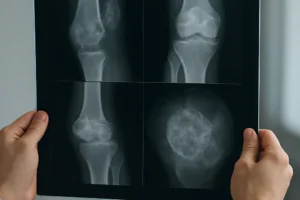
- Imaging: MRI offers superior sensitivity for early marrow changes, while CT provides detailed cortical assessment. Dual-energy X-ray absorptiometry measures density but lacks specificity for infection.
- Laboratory markers: Elevated ESR, CRP, and procalcitonin signal ongoing chronic inflammation. Bone turnover markers, like alkaline phosphatase, may be altered.
- Biopsy and culture: Bone biopsy remains the gold standard for pathogen identification; molecular techniques such as PCR enhance detection of fastidious organisms.
- Advanced techniques: PET-CT and labeled leukocyte scans improve localization of infectious foci in complex cases.
An integrated approach combining imaging, serology, and targeted sampling yields the highest diagnostic yield while guiding personalized treatment.
Therapeutic Strategies
Management of infection-induced bone loss requires a multidisciplinary approach to eradicate pathogens and restore integrity. Core components include:
- Antimicrobial therapy: tailored regimens based on microbial sensitivity, with consideration of bone penetration and biofilm activity.
- Surgical intervention: debridement of necrotic tissue, abscess drainage, and stabilization using internal or external fixation when required.
- Adjunctive treatments: bisphosphonates and denosumab may inhibit osteoclastic activity, but their use in active infection remains controversial. Anabolic agents like teriparatide show promise for enhancing bone formation.
- Immunomodulation: targeting key cytokines (e.g., TNF inhibitors) can mitigate destructive inflammation, although infection control must be ensured prior to therapy.
- Rehabilitation: physical therapy and nutritional support facilitate functional recovery and optimize skeletal health.
Long-term follow-up is essential to monitor for relapse, assess bone density, and adjust treatment plans to maintain an optimal balance between antimicrobial control and bone remodeling.