Bone health in postmenopausal women is a complex interplay of hormonal, nutritional, and lifestyle factors that affects quality of life and long-term functional independence. Following the decline in ovarian function, women encounter a rapid decrease in bone mass and changes in bone architecture, heightening the risk of fragility fractures. Understanding the underlying mechanisms, identifying risk factors, and implementing appropriate therapeutic interventions are essential to mitigate the burden of osteoporosis and related complications in this population.
Physiological Changes and Pathophysiology
During the menopausal transition, the ovaries produce significantly less estrogen, a hormone that plays a vital role in maintaining the balance between bone formation by osteoblasts and bone resorption by osteoclasts. Loss of estrogen leads to:
- Accelerated bone turnover, with resorption outpacing formation
- Reduction in b one mineral density (BMD)
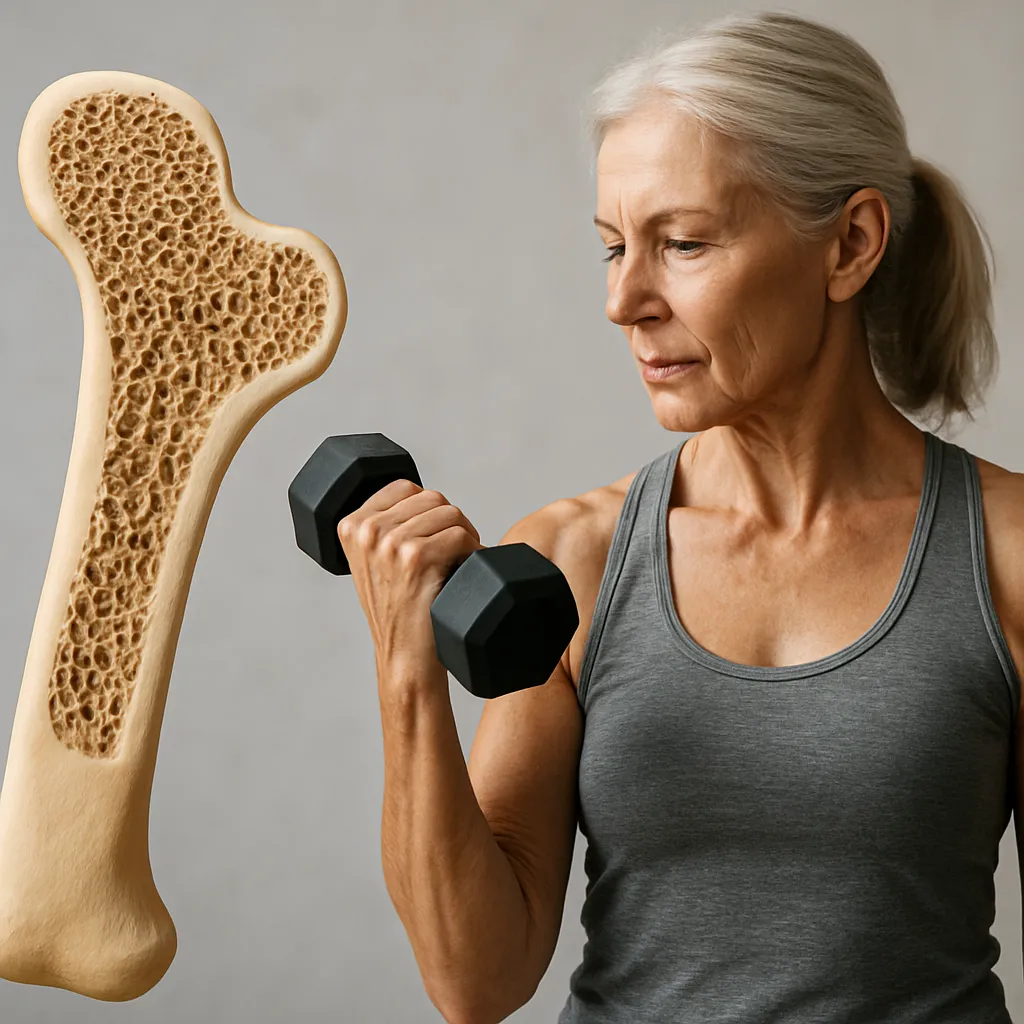
- Changes in trabecular microarchitecture and cortical thinning
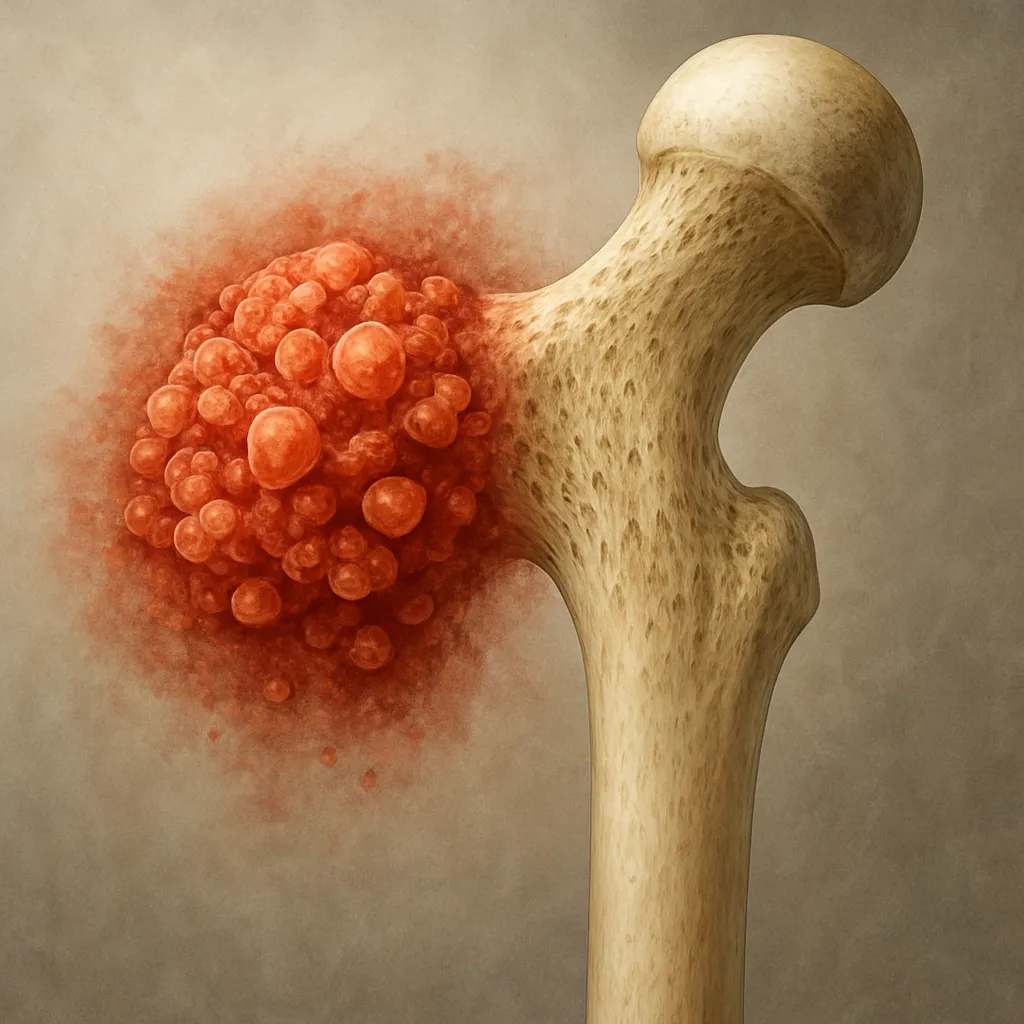
These alterations compromise bone strength, making skeletal structures more susceptible to microdamage and fractures. Additionally, estrogen deficiency can increase inflammatory cytokines such as interleukin-6 (IL-6), which further stimulates osteoclastic activity.
Role of Bone Remodeling Units
Within basic multicellular units (BMUs), coordinated activity between osteoclasts and osteoblasts is critical. Diminished estrogen skews this balance:
- Osteoclastogenesis is promoted via RANKL upregulation
- Osteoprotegerin (OPG) levels decline, reducing protective effects
- Net bone loss accelerates, particularly in trabecular compartments
Major Risk Factors Affecting Bone Health
Beyond hormonal changes, several intrinsic and extrinsic factors influence skeletal integrity in postmenopausal women:
- Age: Bone loss continues progressively with advancing years
- Genetic predisposition: Family history of osteoporosis or fractures
- Calcium and vitamin D deficiency: Impairment in mineralization
- Physical inactivity: Reduced mechanical loading weakens bone
- Excessive alcohol and tobacco use: Toxic to osteoblasts and hinders calcium absorption
- Use of glucocorticoids or other medications affecting bone metabolism
- Low body mass index (BMI) and inadequate nutritional status
Identifying these factors early through clinical history and screening protocols can enable timely intervention.
Diagnostic and Monitoring Tools
Accurate assessment of bone health is fundamental to risk stratification and management. Available modalities include:
Dual-Energy X-ray Absorptiometry (DXA)
- Gold standard for measuring bone mineral density at the lumbar spine, femoral neck, and total hip
- T-score interpretation: Normal (> –1), Osteopenia (–1 to –2.5), Osteoporosis (< –2.5)
- Repeat scans every 1–2 years for monitoring therapeutic response
Quantitative Ultrasound and Peripheral QCT
- Useful in settings where DXA is unavailable
- Provides information on bone quality and microarchitecture
Laboratory Biomarkers
- Bone turnover markers such as serum C-terminal telopeptide (CTX) and bone-specific alkaline phosphatase (BSAP)
- 25-hydroxyvitamin D, calcium, parathyroid hormone (PTH) levels
- Assessment of secondary causes: thyroid function, renal profile, celiac screening
Therapeutic Approaches
An individualized treatment plan aims to reduce fracture risk by enhancing bone strength and minimizing resorption. Treatment categories include:
Anti-Resorptive Agents
- Bisphosphonates: Alendronate, risedronate, zoledronic acid; inhibit osteoclast-mediated resorption
- Denosumab: Monoclonal antibody against RANKL, reversible upon discontinuation
- Selective estrogen receptor modulators (SERMs): Raloxifene reduces vertebral fracture risk
Anabolic Therapies
- Teriparatide: Recombinant PTH enhances bone formation; limited duration of use
- Abaloparatide: PTH-related peptide analog with bone-building effects
Hormone Replacement Therapy (HRT)
While HRT can preserve bone mass and alleviate menopausal symptoms, it requires careful consideration of cardiovascular and oncological risks. Lower-dose regimens may be suitable for women under 60 within 10 years of menopause onset.
Lifestyle and Nutritional Strategies
Complementary measures play a pivotal role in optimizing bone health:
- Calcium intake: Daily intake of 1,000–1,200 mg from diet and supplements
- Vitamin D supplementation: Aim for serum 25(OH)D levels ≥30 ng/mL
- Weight-bearing and resistance exercises to stimulate remodeling and increase muscle strength
- Fall prevention strategies: balance training, home safety evaluations
- Smoking cessation and moderation of alcohol consumption
Multidisciplinary collaboration involving endocrinologists, primary care providers, dietitians, and physiotherapists enhances the effectiveness of bone health programs and addresses coexisting health concerns.