Bone lesions encompass a diverse spectrum of conditions, ranging from benign abnormalities to aggressive neoplasms. Accurate identification and characterization of these lesions are crucial for determining prognosis and guiding treatment. Imaging plays an indispensable role in this process, offering insights into lesion composition, biological activity, and potential systemic involvement. This article examines the underlying mechanisms of bone lesions, reviews key imaging modalities, outlines characteristic radiologic patterns, and discusses contemporary diagnostic strategies and innovations.
Pathophysiology and Classification of Bone Lesions
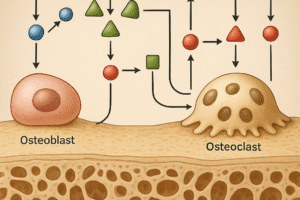
Bone lesions originate from various cellular processes that disrupt normal skeletal homeostasis. In healthy bone, a tightly regulated balance exists between osteoclast-mediated resorption and osteoblast-driven formation. Disruption of this equilibrium can result in focal areas of destruction or excessive bone deposition. Primary bone tumors develop within the skeletal system itself, whereas secondary or metastatic lesions arise when malignant cells spread from distant organs.
Broadly, bone lesions are classified as:
- Benign lesions such as osteochondromas, enchondromas, and osteoid osteomas that typically exhibit well-defined margins, slow growth, and limited clinical aggressiveness.
- Malignant primary tumors including osteosarcoma, Ewing sarcoma, and chondrosarcoma, which often demonstrate rapid expansion, cortical breach, and soft tissue extension.
- Metastatic involvement where carcinoma cells—commonly from breast, prostate, lung, or kidney—invade bone, producing lesions that may be osteolytic, osteoblastic, or mixed in appearance.
- Infectious or inflammatory conditions like osteomyelitis, which mimic tumor-like processes through bone destruction and reactive sclerosis.
The biological behavior of each lesion type is influenced by molecular signaling pathways. For instance, upregulation of RANKL (Receptor Activator of Nuclear factor Kappa-Β Ligand) drives osteoclast activation in lytic lesions, whereas aberrant BMP (Bone Morphogenetic Protein) signaling contributes to abnormal osteoid production in sclerotic tumors. Understanding these mechanisms provides a foundation for targeted therapies and emerging molecular imaging techniques.
Imaging Modalities and Techniques
A multimodality approach enhances diagnostic accuracy by combining the strengths of different imaging technologies. Each modality offers unique advantages in assessing bone architecture, lesion matrix, vascularization, and metabolic activity.
Plain Radiography
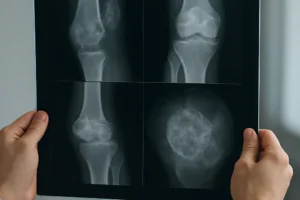
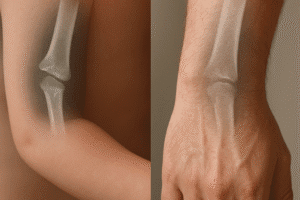
Standard X-ray remains the initial screening tool. It efficiently reveals cortical integrity, periosteal reaction, and gross matrix patterns. Key radiographic features include:
- Lesion margins: Narrow, sclerotic rim suggests a benign process; ill-defined borders raise suspicion for high-grade malignancy.
- Periosteal response: Lamellated or sunburst patterns often correlate with aggressive tumor growth.
- Matrix mineralization: Chondroid rings-and-arcs versus osteoid cloud-like densities.
Computed Tomography (CT)
CT scanning offers superior depiction of cortical destruction, matrix mineralization, and small calcifications. High-resolution reconstructions facilitate surgical planning by delineating lesion extent and involvement of neurovascular structures. Contrast-enhanced CT may highlight hypervascular tumors and guide percutaneous biopsy.
Magnetic Resonance Imaging (MRI)
MRI excels in soft tissue contrast and marrow evaluation. T1-weighted images distinguish fatty marrow replacement, while T2-weighted and STIR sequences highlight edema and tumor infiltration. Contrast-enhanced fat-suppressed sequences further delineate viable tumor from necrosis. MRI is indispensable for local staging and assessing skip lesions.
Nuclear Medicine and Functional Imaging
Bone scintigraphy using technetium-99m-labeled phosphonates offers whole-body screening for multifocal disease. Positron emission tomography (PET) with 18F-FDG or newer tracers such as 18F-NaF provides quantitative data on glucose metabolism or osteoblastic activity. Integration of PET with CT (PET/CT) or MRI (PET/MRI) refines lesion localization and characterization.
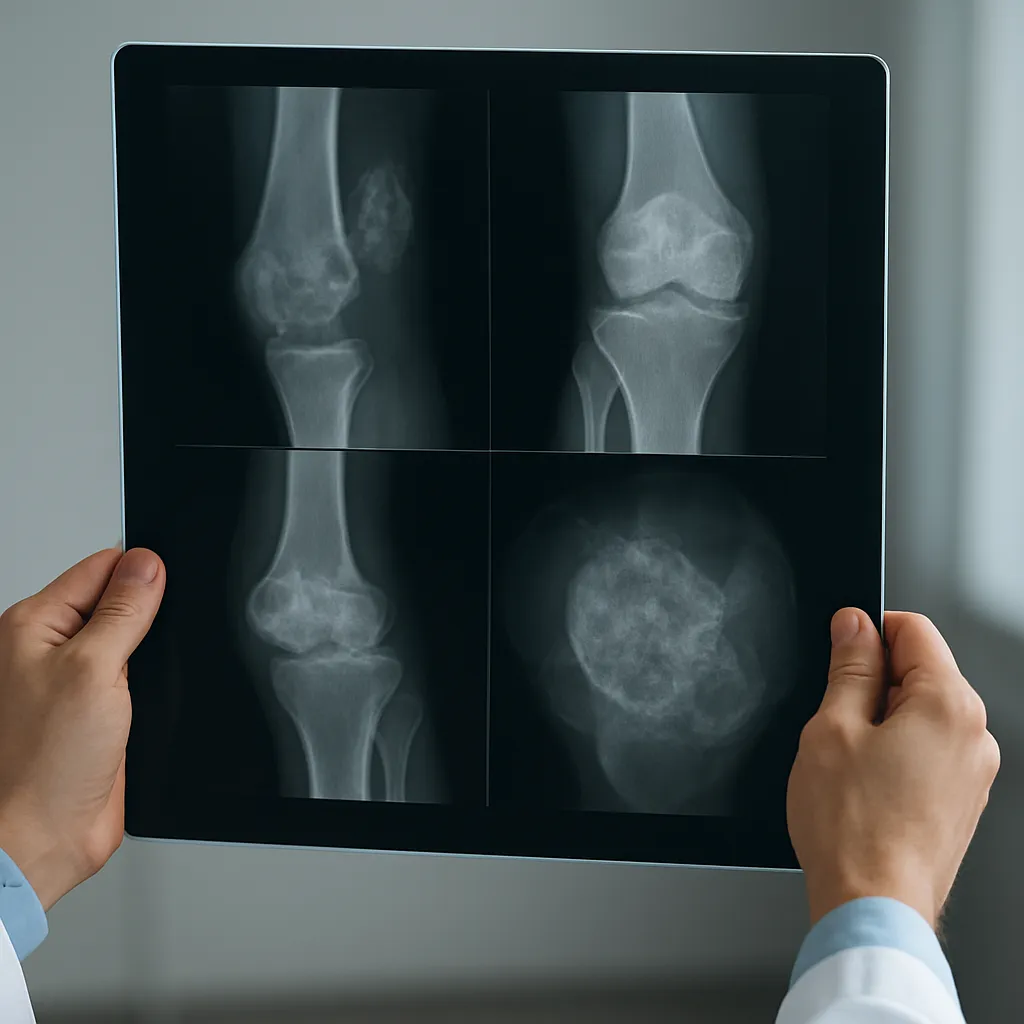
Radiologic Patterns and Differential Diagnosis
Recognizing imaging patterns enables a targeted differential diagnosis. Key radiologic appearances include:
- Osteolytic lesions: Characterized by bone resorption and radiolucency. Common in metastases from lung, kidney, and thyroid primaries. Primary tumors such as multiple myeloma also present this way.
- Osteoblastic lesions: Marked by sclerotic new bone formation. Typical of prostate cancer metastases and osteosclerotic variants of lymphoma.
- Mixed lytic-sclerotic lesions: Seen in breast cancer metastases, Paget disease, and certain sarcomas.
- Geographic defects with sclerotic margins: Suggest slow-growing benign lesions like bone cysts or fibrous dysplasia.
The differential diagnosis should consider clinical context, patient age, lesion location, and associated symptoms such as pain, systemic signs, or pathological fracture. For example:
- A diaphyseal lytic lesion in a child with periosteal elevation raises suspicion for Ewing sarcoma.
- An epiphyseal lesion with chondroid calcification in a young adult suggests an enchondroma or chondrosarcoma.
- Multiple sclerotic foci in an elderly man point toward prostate cancer metastasis.
Diagnostic Workflow and Emerging Trends
The evaluation of bone lesions follows a structured workflow:
- Comprehensive clinical assessment including history, laboratory tests (alkaline phosphatase, tumor markers), and symptom evaluation.
- Initial radiographs to localize and characterize lesions.
- Advanced imaging (CT, MRI, PET) tailored to lesion features and clinical concerns.
- Image-guided biopsy for histopathological confirmation and molecular profiling.
Recent advances are transforming the field. Radiomics extracts high-dimensional data from images to predict tumor phenotype and treatment response. Artificial intelligence algorithms enhance lesion detection and classification, reducing diagnostic delays. Novel radiotracers enable specific targeting of molecular receptors, while hybrid PET/MRI scanners combine metabolic and morphological information in a single session. In parallel, minimally invasive ablative therapies guided by imaging are offering new treatment avenues for select patients.
Effective management of bone lesions demands a multidisciplinary approach involving radiologists, orthopedic surgeons, pathologists, and oncologists. Continued innovation in imaging technology and data analysis holds promise for more precise diagnosis, personalized therapy, and improved patient outcomes.