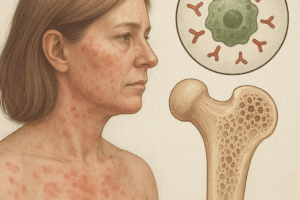
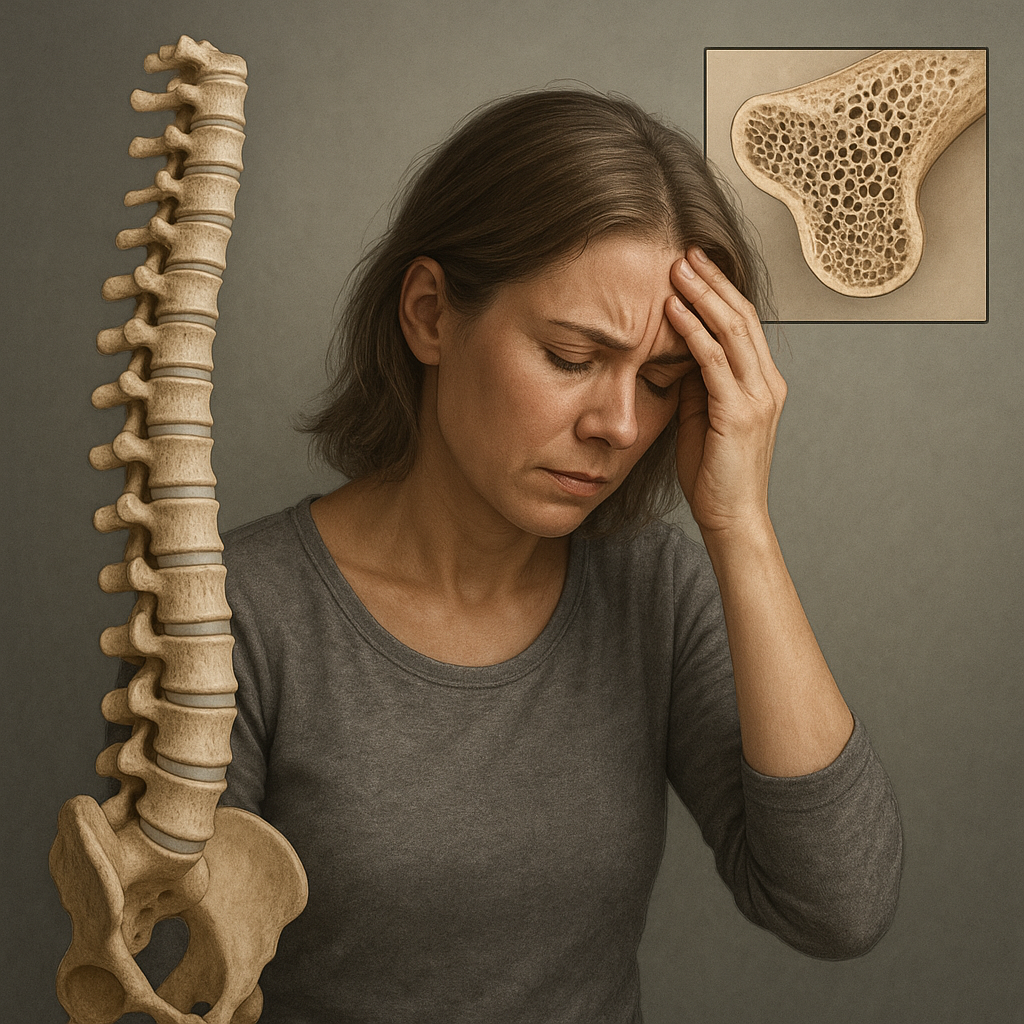
The intricate balance of bone formation and resorption can be profoundly disrupted by persistent psychological pressures. Chronic stress, often dismissed as purely mental, exerts systemic effects that compromise the health of the skeletal framework. By unraveling the **biological**, **clinical**, and **therapeutic** dimensions, this article explores how long-term stress undermines bone integrity and outlines strategies to safeguard skeletal well-being.
Biological Mechanisms Linking Chronic Stress and Bone Integrity
Hypothalamic-Pituitary-Adrenal Axis Dysregulation
Chronic activation of the **HPA** axis leads to sustained elevations of **cortisol**, a glucocorticoid hormone that plays a central role in stress adaptation. Elevated cortisol:
- Suppresses osteoblast proliferation and differentiation, reducing bone **formation**.
- Enhances osteoclast lifespan and activity, accelerating **resorption**.
- Impairs intestinal **calcium** absorption and increases urinary calcium excretion, depleting mineral reserves.
This hormonal milieu skews the normal bone **remodeling** cycle, tipping the balance toward net bone loss.
Sympathetic Nervous System and Neurotransmitter Effects
Persistent stress triggers sympathetic overdrive, releasing **catecholamines** like adrenaline and noradrenaline. These neurotransmitters bind to β-adrenergic receptors on bone cells, leading to:
- Reduced osteoblast activity due to cyclic AMP signaling alterations.
- Enhanced osteoclastogenesis mediated by RANKL upregulation.
- Vascular constriction in bone microcirculation, compromising nutrient delivery to bone tissue.
The chronic sympathetic tone fosters an environment where **bone density** progressively declines.
Inflammatory Mediators and Bone Remodeling
Stress-induced immune dysregulation elevates pro-inflammatory cytokines such as **IL-6**, **TNF-α**, and IL-1β. These molecules:
- Stimulate osteoclast precursors, increasing bone **catabolism**.
- Inhibit osteoblast **matrix** production and mineralization.
- Contribute to systemic low-grade inflammation that persists over time.
The interplay between the immune and skeletal systems underscores the concept of the “osteoimmunological” axis, where immune overactivation accelerates bone deterioration.
Clinical Consequences of Prolonged Stress on Skeletal System
Osteoporosis and Fracture Risk
Long-term stress correlates with reduced bone mineral density (BMD) in both trabecular and cortical compartments. Clinicians observe:
- Higher prevalence of **osteopenia** and osteoporosis in individuals with chronic anxiety or depressive disorders.
- Increased incidence of vertebral and non-vertebral **fractures**, even with minimal trauma.
- Delayed peak bone mass acquisition in adolescents experiencing prolonged stress.
These trends underscore the importance of early detection of stress as a modifiable risk factor in **skeletal** fragility assessments.
Impact on Bone Healing and Regeneration
Bone repair after injury or surgery relies on coordinated inflammatory, proliferative, and remodeling phases. Chronic stress disrupts each phase by:
- Prolonging inflammation via sustained cytokine release, delaying the transition to repair.
- Reducing mesenchymal stem cell recruitment and differentiation into osteoblasts.
- Altering angiogenesis, thereby limiting vascular support for new bone tissue.
Consequently, fracture healing may be significantly slower, with an elevated risk of **nonunion** and compromised mechanical strength.
Interactions with Comorbid Conditions
Chronic stress often coexists with behavioral and metabolic disorders—smoking, alcohol abuse, poor nutrition, and diabetes—all of which compound skeletal risks. For instance:
- Nicotine impairs osteoblast function and promotes oxidative stress in bone microenvironment.
- Excess alcohol increases parathyroid hormone secretion, leading to secondary hyperparathyroidism.
- Poor glycemic control in diabetes hinders collagen cross-linking, compromising bone quality despite normal BMD.
These comorbidities demand a holistic approach to patient evaluation and management.
Strategies for Mitigating Stress-Related Bone Deterioration
Pharmacological Approaches
Targeted medications can counteract the skeletal effects of stress:
- Bisphosphonates and denosumab inhibit osteoclast-mediated **resorption**, preserving BMD.
- Selective glucocorticoid receptor modulators may dissociate anti-inflammatory actions from bone catabolic effects.
- SSRIs and SNRIs help manage **depressive** symptoms, indirectly reducing HPA axis hyperactivity.
Optimizing medication regimens requires balancing psychiatric and skeletal needs to minimize adverse outcomes.
Lifestyle and Behavioral Interventions
Non-pharmacological strategies play a pivotal role in protecting bone health under chronic stress:
- Regular weight-bearing and resistance **exercise** stimulates osteogenesis through mechanical loading.
- Mindfulness, yoga, and cognitive behavioral therapy (CBT) modulate stress perception and lower cortisol levels.
- Balanced diet rich in calcium, vitamin D, and protein supports bone matrix formation and mineralization.
- Sleep hygiene improves endogenous growth hormone secretion, vital for bone **repair**.
Comprehensive programs integrating exercise, nutrition, and stress reduction offer the most robust defense against stress-induced bone loss.
Emerging Therapies and Research Directions
Ongoing studies are evaluating novel interventions:
- Gut microbiome modulation to enhance calcium absorption and reduce systemic inflammation.
- Peptide hormones such as osteocalcin analogs to stimulate osteoblast activity.
- Gene-targeted therapies aiming to normalize RANK/RANKL/OPG signaling in stressed individuals.
Translational research holds promise for tailored treatments that address the multi-system impact of chronic stress on bone health.