Bone regenerative medicine has transformed the landscape of orthopedics by integrating cutting-edge technologies and biological insights to restore skeletal integrity. Recent developments have focused on harnessing the body’s innate repair mechanisms, engineering advanced materials, and optimizing cellular therapies. This article explores the latest innovations driving progress in bone healing and reconstruction, highlighting key strategies that promise to redefine patient outcomes.
Emerging Biomaterials for Bone Repair
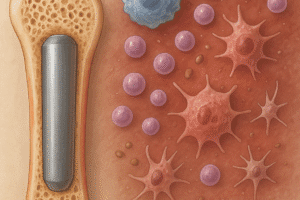
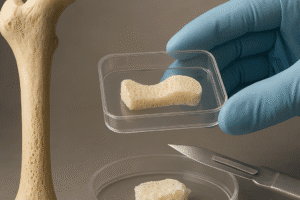
The choice of biomaterials is fundamental to guiding new bone formation. Recent years have seen a surge in hybrid composites combining natural polymers, ceramics, and synthetic matrices. These materials aim to replicate the complex architecture and mechanical resilience of native bone.
- Scaffolds based on calcium phosphate ceramics exhibit high osteoconductivity, providing a structural framework for osteogenesis.
- Bioactive glasses release ionic species that stimulate cellular proliferation and matrix deposition.
- Composite hydrogels incorporate collagen and chitosan to enhance biocompatibility and controlled degradation.
Advances in nanotechnology have enabled the fabrication of nanofibrous scaffolds with pore sizes tailored to cell infiltration and nutrient exchange. Surface functionalization with peptides and growth factors further directs stem cell attachment and differentiation. Researchers have also investigated photocrosslinkable polymers that solidify in situ under safe light exposure, allowing minimally invasive implantation.
Stem Cell and Growth Factor Strategies
Mesenchymal Stem Cell Therapies
Mesenchymal stem cells (MSCs) are multipotent progenitors capable of differentiating into osteoblasts, chondrocytes, and adipocytes. Their immunomodulatory properties and trophic factor secretion make them ideal candidates for bone regeneration. Clinical protocols now employ MSCs sourced from bone marrow, adipose tissue, or umbilical cord blood.
Preconditioning MSCs with mechanical stimuli or hypoxia enhances their pro-angiogenic and osteoinductive potential. Genetic modification to overexpress osteogenic transcription factors further accelerates matrix mineralization. Encapsulation within biodegradable microcarriers facilitates targeted delivery and sustained viability at the defect site.
Growth Factor Delivery Systems
Growth factors such as bone morphogenetic proteins (BMPs), vascular endothelial growth factor (VEGF), and platelet-derived growth factor (PDGF) are critical signals for bone repair. Direct administration, however, often leads to rapid diffusion and adverse side effects. To overcome these challenges, researchers have developed controlled-release platforms:
- Layer-by-layer coatings on implant surfaces for sequential factor release.
- Injectable microparticles encapsulating BMP-2 in a polymer matrix.
- Electrospun fibers loaded with VEGF to promote early angiogenesis.
Synergistic combinations of growth factors delivered in a spatially and temporally regulated manner mimic natural healing cascades, leading to higher quality bone and faster recovery.
Advanced Technologies and Clinical Applications
The convergence of biofabrication, genetic engineering, and real-time imaging has ushered in an era of personalized bone constructs. 3D bioprinting enables the precise deposition of cells and biomaterials in complex geometries matching patient-specific defect anatomy. Bioinks formulated with MSCs and calcium phosphate particles have successfully generated trabecular-like structures in preclinical models.
Gene Therapy Approaches
Gene therapy offers a means to achieve sustained local production of osteogenic factors. Viral and nonviral vectors deliver DNA encoding for BMPs or Runx2 directly into host cells. Advances in CRISPR/Cas9 technology allow for site-specific genomic edits, potentially correcting hereditary bone disorders or upregulating endogenous repair genes. Safety and off-target effects remain active areas of investigation, with several clinical trials underway to evaluate efficacy in nonunion fractures.
Exosome-Based Regeneration
Exosomes, nanoscale vesicles secreted by cells, carry proteins, RNAs, and lipids that modulate recipient cell behavior. MSC-derived exosomes have demonstrated potent osteoinductive and immunoregulatory effects without the risks associated with cell transplantation. Encapsulation of exosomes within hydrogels or coating them onto titanium implants has led to enhanced bone deposition and reduced inflammation in animal studies.
Translational Challenges and Future Directions
While numerous strategies show promise, translating laboratory successes to clinical practice demands rigorous evaluation. Standardizing manufacturing processes for cell therapies, ensuring batch-to-batch consistency of biomaterials, and establishing long-term safety profiles are crucial steps. Regulatory frameworks must evolve to accommodate complex combination products that integrate cells, genes, and devices.
Interdisciplinary collaboration among bioengineers, molecular biologists, and clinicians is driving the innovation pipeline. Artificial intelligence tools are now being applied to predict scaffold performance, optimize bioprinting parameters, and design personalized treatment plans. As these efforts converge, the vision of fully functional, patient-tailored bone grafts moves closer to reality, offering hope for those with large defects, osteoporosis-related fractures, and congenital skeletal anomalies.