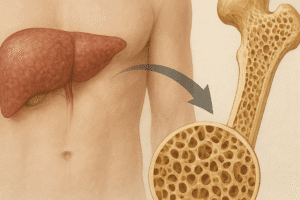
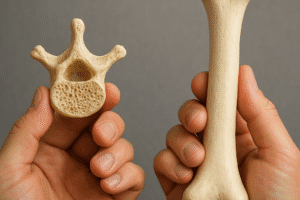
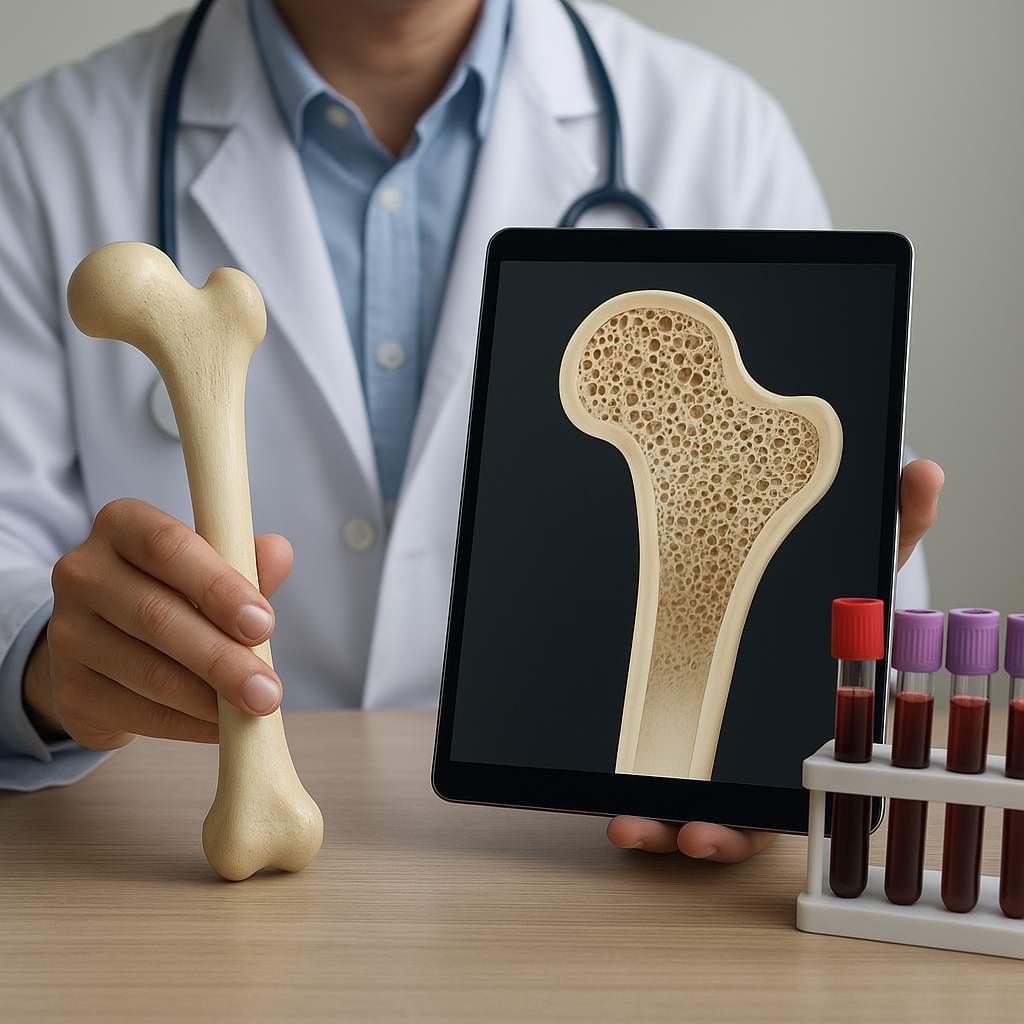
Bone is a remarkably dynamic organ that not only provides structural support but also serves as a vital reservoir for essential minerals. Recent investigations in bone biology have unveiled intricate molecular networks and novel therapeutic strategies aimed at enhancing skeletal strength and repair. This article explores groundbreaking findings in cellular dynamics, stem cell–based therapies, mechanobiology, and clinical translation, offering insights into future directions for improving bone health.
Understanding the Cellular Dynamics of Bone Remodeling
Bone tissue constantly undergoes a remodeling process orchestrated by two primary cell types: the osteoblast, responsible for new matrix formation, and the osteoclast, which resorbs old or damaged bone. This delicate balance of bone remodeling relies on a network of signaling pathways, including RANK/RANKL/OPG, Wnt/β-catenin, and Notch. Disruption of these cascades can lead to skeletal disorders such as osteoporosis or osteopetrosis.
Recent studies have shed light on the role of inflammatory cytokines (e.g., TNF-α, IL-6) in modulating osteoclastogenesis. Advanced imaging techniques, like two-photon microscopy, have visualized how osteoclasts traverse the bone surface, creating resorption lacunae. Meanwhile, single-cell RNA sequencing has identified subpopulations of osteolineage cells with unique gene signatures, revealing previously unrecognized intermediates in the differentiation trajectory from mesenchymal progenitors to mature osteoblasts.
Emerging evidence highlights the influence of the skeletal niche’s microenvironment. The cross-talk between endothelial cells and bone cells via angiogenic factors (VEGF, PDGF) underscores the coupling of angiogenesis and osteogenesis. Targeting these interactions has shown promise in animal models, where local delivery of VEGF analogues enhances vascularization and accelerates bone repair. Additionally, the discovery of perivascular skeletal stem cells challenges traditional views, positioning vascular walls as reservoirs of osteoprogenitors.
Advances in Stem Cell–Based Therapies for Bone Repair
The quest for effective bone regeneration has propelled research into stem cells. Mesenchymal stem cells (MSCs), derived from bone marrow, adipose tissue, or umbilical cord, exhibit multipotency and immunomodulatory properties. Preclinical models demonstrate that transplanting MSCs into critical-sized defects fosters robust bone formation, particularly when combined with osteoinductive factors like BMP-2.
Scaffold Design and Biomaterials
Integration of MSCs with advanced biomaterials has revolutionized scaffold-based strategies. Biodegradable polymers (PLGA, PCL) and bioactive ceramics (hydroxyapatite, tricalcium phosphate) provide structural support while releasing growth factors in a controlled manner. Novel approaches employ 3D bioprinting to create patient-specific constructs that mimic the hierarchical architecture of native bone. Incorporating nano-scale features enhances cell adhesion and differentiation, optimizing the regeneration process.
Gene Editing and Precision Medicine
CRISPR/Cas9 technology offers avenues to enhance MSC osteogenic potential by upregulating bone-promoting genes (e.g., RUNX2, BMP receptors) or silencing inhibitors (e.g., DKK1). Customizing cell therapies through gene editing aligns with the principles of precision medicine, tailoring interventions to individual genetic profiles. Early-phase clinical trials are exploring engineered MSCs for nonunion fractures and osteoporosis, reporting encouraging safety and efficacy outcomes.
Mechanobiology: The Role of Mechanical Forces in Bone Health
Bone’s ability to sense and adapt to mechanical loads is crucial for maintaining mass and architecture. The field of mechanotransduction investigates how cells convert physical stimuli into biochemical signals. Primary cilia, integrins, and stretch-activated ion channels (Piezo1) act as mechanosensors driving anabolic responses. In vitro studies reveal that cyclic strain enhances osteoblast proliferation, while fluid shear stress stimulates osteocyte secretion of sclerostin antagonists, promoting bone formation.
Microgravity experiments onboard the International Space Station have provided unique insights. Astronauts experience rapid bone loss in weight-bearing regions due to reduced mechanical loading. Analysis of bone biopsies post-flight shows decreased osteoblast activity and altered gene expression patterns related to Wnt signaling. These findings inform countermeasures for osteoporosis on Earth, such as targeted vibration therapy or mechanical stimulation devices designed to mimic gravitational forces at the cellular level.
Sports science also contributes to mechanobiology. High-impact exercises, like jumping or resistance training, generate peak strains that signal osteogenesis. Computational modeling integrates strain distribution data with bone adaptation laws, predicting sites at risk for stress fractures or optimal loading regimens to enhance bone strength in aging populations. Wearable sensors now allow continuous monitoring of activity patterns and load magnitudes, linking real-world data to personalized exercise prescriptions.
Translational Research and Clinical Applications
Bridging laboratory discoveries to patient care has accelerated thanks to multidisciplinary collaborations. Novel pharmacologic agents targeting sclerostin (e.g., romosozumab) have entered clinical practice, offering dual anabolic and antiresorptive effects. Ongoing trials evaluate combination therapies, such as pairing sclerostin inhibitors with low-dose parathyroid hormone analogues, to maximize bone accrual while minimizing adverse events.
- Minimally Invasive Techniques: Image-guided delivery of osteoinductive materials enables precise augmentation of vertebral bodies or long-bone defects, reducing surgical morbidity.
- Biomarker Discovery: Circulating microRNAs and extracellular vesicles are under investigation as early indicators of fracture risk or treatment response, enhancing monitoring in osteoporosis management.
- Regenerative Orthopedics: Autologous platelet-rich plasma and bone marrow aspirate concentrate harness endogenous growth factors to stimulate repair in tendinopathies and delayed unions.
Future directions emphasize integrating big data analytics and artificial intelligence to unravel complex bone–organ interactions. Machine learning algorithms can predict fracture outcomes based on patient-specific parameters, guiding tailored interventions. Additionally, wearable technology and telemedicine platforms will enable remote monitoring of therapy adherence and functional recovery, expanding access to bone health services.