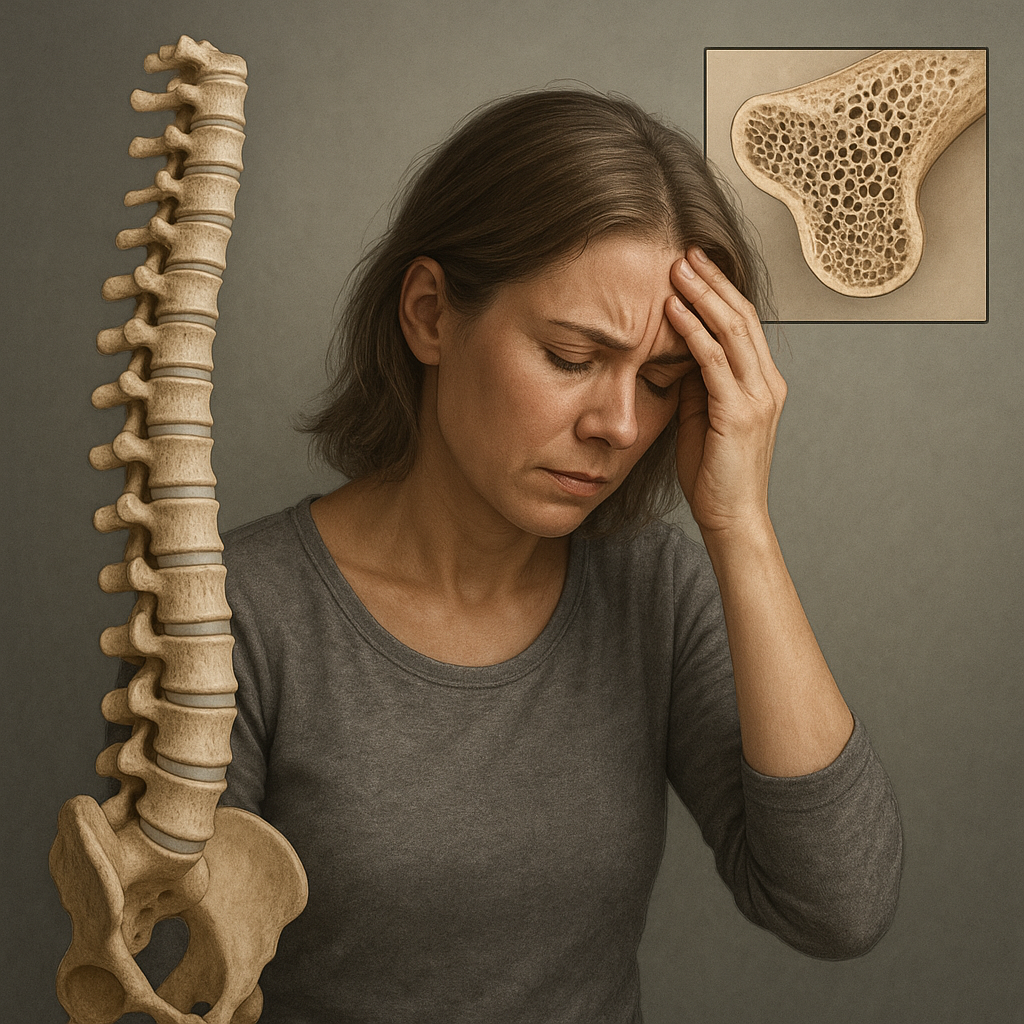
The role of gut health in skeletal integrity has garnered significant attention in recent years. Emerging research highlights the capacity of probiotics to influence bone metabolism through complex interactions within the microbiome. Understanding these processes opens new avenues for addressing bone disorders and improving overall bone density.
Probiotics and the Gut-Bone Axis
The concept of a gut-bone axis refers to the bidirectional communication between the intestinal environment and the skeletal system. The gut harbors trillions of microorganisms whose metabolic byproducts can enter systemic circulation, impacting distant tissues. Probiotics—live microbial supplements—can modulate the composition and function of these resident communities. By enhancing the production of SCFAs (short-chain fatty acids) and fortifying the gut barrier, probiotics reduce systemic inflammation that otherwise contributes to bone resorption.
Healthy bones depend on a delicate balance between bone-forming osteoblasts and bone-resorbing osteoclasts. Dysbiosis—a disrupted microbial state—can tilt this balance towards increased osteoclast activity. Probiotics help restore equilibrium by promoting anti-resorptive signaling pathways, ultimately supporting bone formation and maintenance.
Animal studies have demonstrated that supplementation with strains such as Lactobacillus rhamnosus GG and Bifidobacterium longum leads to measurable improvements in trabecular microarchitecture. The observed increases in bone mineral content correlate with reduced markers of bone turnover, suggesting a direct influence of probiotic-driven metabolites on skeletal cells.
Mechanisms of Action on Bone Metabolism
Probiotics employ multiple mechanisms to exert their osteoprotective effects. These can be grouped into three major categories: immune modulation, nutrient absorption enhancement, and direct cellular signaling.
Immune Modulation
- Probiotics induce regulatory T-cell expansion, reducing pro-inflammatory cytokines such as TNF-α and IL-6.
- Decreased inflammation inhibits excessive osteoclastogenesis, preserving bone structure.
By shifting the immune response toward a more anti-inflammatory profile, probiotics indirectly favor osteoblast activity and matrix deposition.
Nutrient Absorption Enhancement
- Certain probiotic strains improve the absorption of calcium and magnesium in the intestine.
- Enhanced vitamin D metabolism ensures adequate mineralization of the bone matrix.
An optimized digestive tract reduces the risk of malabsorption syndromes that compromise skeletal health, especially in populations prone to deficiencies.
Direct Cellular Signaling
- Probiotic-secreted metabolites can interact with G-protein coupled receptors on osteoblasts.
- These interactions upregulate osteogenic genes such as RUNX2 and OCN.
Through these pathways, probiotics effectively increase the bioavailability of signals that drive bone formation, demonstrating a capacity for direct skeletal support beyond systemic immune effects.
Clinical Evidence and Future Directions
Human trials exploring probiotic supplementation have yielded promising outcomes for bone health. In peri- and postmenopausal women, daily intake of specific Lactobacillus strains resulted in significant reductions in bone resorption markers over a six-month period. Adolescents with low bone mass who received a multistrain probiotic supplement showed improvements in lumbar spine bone mineral density as measured by DXA scans.
Despite these encouraging findings, larger randomized controlled studies are needed to establish standardized dosing regimens and identify the most effective strains. The variability in individual microbiome profiles suggests that personalized probiotic therapy could become a reality in the near future.
Innovative approaches such as synbiotics—combinations of prebiotics and probiotics—are under investigation for their synergistic effects. These formulations may further enhance nutrient absorption and immune modulation, delivering a potent one-two punch against osteoporosis.
Future research is likely to explore multiomics analyses that integrate metagenomics, metabolomics, and host gene expression. Such comprehensive datasets will illuminate the precise molecular dialogues between microbes and bone cells, facilitating targeted interventions.
Moreover, the development of next-generation probiotics, including genetically engineered strains, holds the potential to deliver therapeutic molecules directly at the intestinal epithelium, maximizing localized effects while minimizing systemic exposure.
As the field advances, collaboration between microbiologists, endocrinologists, and bioinformaticians will be crucial. Integrating clinical insights with computational modeling can accelerate the translation of basic research into effective, evidence-based treatments for maintaining lifelong skeletal health.