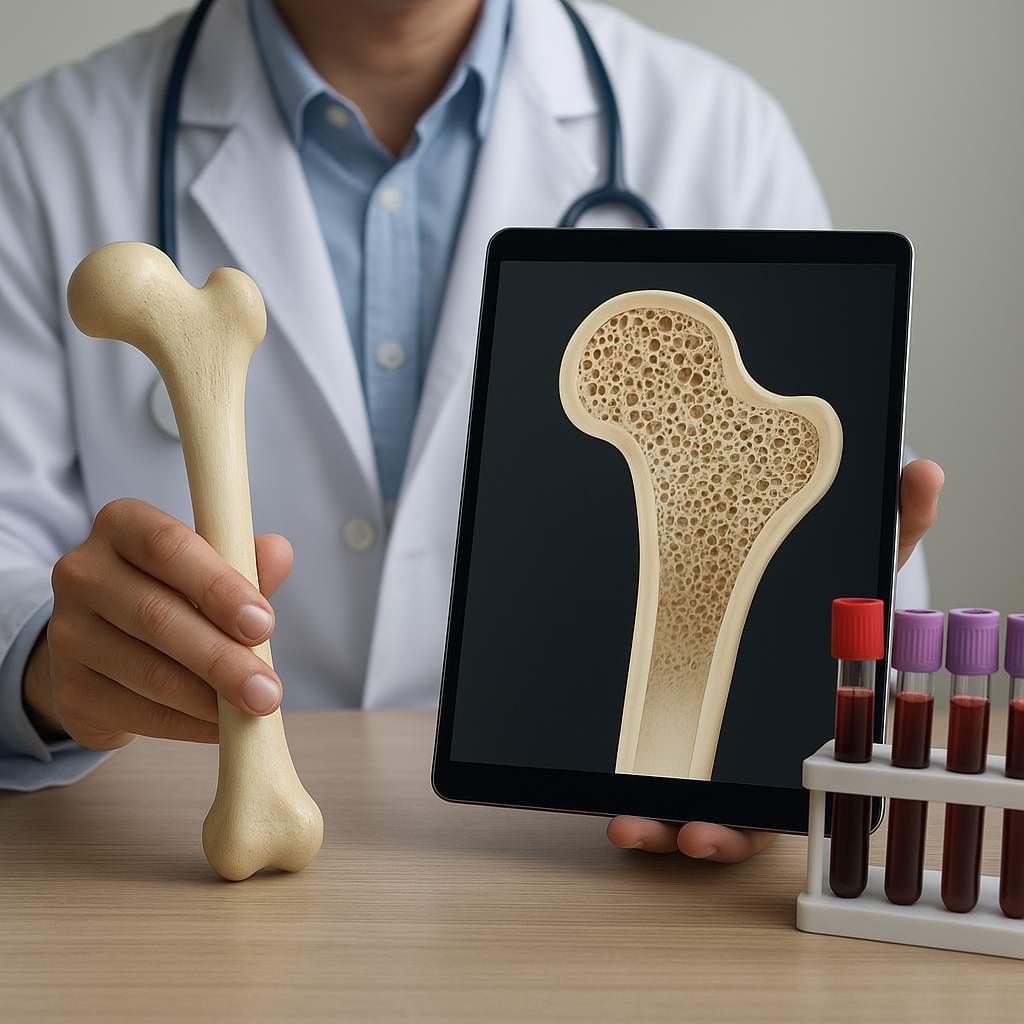
The regulation of bone turnover by Parathyroid Hormone (PTH) represents a complex interplay of cellular, molecular, and systemic processes that maintain skeletal integrity and calcium homeostasis. Secreted from the parathyroid glands in response to declining serum calcium levels, PTH acts on bone, kidney, and the intestine to orchestrate a balanced cycle of resorption and formation. An in-depth understanding of these mechanisms provides critical insights for the development of novel therapies targeting osteoporosis, fracture healing, and other metabolic bone diseases. This article explores the physiology, cellular pathways, clinical applications, and future directions in PTH-mediated bone remodeling.
Physiology of Parathyroid Hormone and Bone Homeostasis
Parathyroid Hormone is an 84–amino acid peptide whose primary function is to restore serum calcium. It binds to a specific G protein–coupled receptor, PTH1R, found on osteoblasts and osteocytes. Upon binding, PTH triggers a cascade of intracellular events that promote bone resorption indirectly by increasing the expression of RANKL (Receptor Activator of Nuclear factor Kappa-Β Ligand) while suppressing osteoprotegerin (OPG). This shift in the RANKL/OPG ratio enhances differentiation and activation of osteoclasts, resulting in release of mineralized calcium and phosphate from the bone matrix.
Simultaneously, PTH exerts effects on renal tubular cells to increase calcium reabsorption and stimulate the conversion of 25-hydroxyvitamin D to its active form, 1,25-dihydroxyvitamin D, which enhances intestinal calcium uptake. The net effect is restoration of extracellular calcium, maintaining a tight physiological range critical for neuromuscular function, blood coagulation, and cellular signaling. The pulsatile nature of PTH secretion—minute-to-minute oscillations—favors bone anabolism when provided intermittently, while continuous elevations lead to catabolism.
Cellular Mechanisms of PTH in Bone Remodeling
PTH Binding and Signal Transduction
When PTH engages PTH1R on osteoblast-lineage cells, it activates heterotrimeric G proteins that stimulate adenylate cyclase, elevating cyclic AMP levels and activating protein kinase A (PKA). Concurrently, alternative pathways involving phospholipase C, protein kinase C, and β-arrestin–mediated signaling contribute to a diversified response profile. This network of pathways converges on transcription factors such as CREB (cAMP response element-binding protein), ultimately regulating genes responsible for matrix turnover and cellular differentiation.
Regulation of Osteoblast and Osteoclast Activity
PTH’s influence on osteoblasts spans promotion of cell survival, proliferation, and matrix synthesis. Intermittent PTH exposure induces anabolic factors such as Insulin-like Growth Factor 1 (IGF-1), osteopontin, and bone morphogenetic proteins, thereby fostering new bone deposition. In contrast, sustained PTH elevation drives osteoblasts to secrete higher levels of RANKL, tipping the balance toward osteoclastogenesis. Osteoclast precursors, expressing the RANK receptor, undergo maturation, attach to the bone surface, and initiate acidification and proteolytic enzyme secretion (e.g., cathepsin K), dissolving hydroxyapatite and collagen matrix.
- Pro-survival signaling: PKA-mediated inhibition of osteoblast apoptosis
- Matrix synthesis: Upregulation of collagen type I and noncollagenous proteins
- Resorption initiation: Activation of tartrate-resistant acid phosphatase in osteoclasts
The dynamic coupling between osteoclast-mediated resorption and osteoblast-driven formation ensures bone remodeling adapts to mechanical stress and mineral demands. Disruption of this coupling underlies pathologies such as primary hyperparathyroidism (continuous PTH) and osteoporosis (net bone loss).
Clinical Implications and Therapeutic Strategies
Leveraging the dual nature of PTH’s effects, clinicians have developed therapeutic regimens that harness its anabolic potential. Teriparatide (PTH[1–34]) and abaloparatide (PTHrP analog) administered intermittently stimulate bone formation, substantially increasing bone mineral density (BMD) and reducing fracture risk in high-risk osteoporotic patients. Treatment protocols typically involve daily subcutaneous injections over 18–24 months, with vigilant monitoring of serum calcium, skeletal markers, and renal function.
Pharmacological Interventions
- Teriparatide: Enhances osteoblast number and activity
- Abaloparatide: Selective PTH1R activation with reduced resorptive signaling
- Combination therapies: Sequential use with antiresorptives (e.g., bisphosphonates, denosumab) to maximize gain
Monitoring and Safety Considerations
Potential adverse effects include transient hypercalcemia, orthostatic hypotension, and injection-site reactions. Long-term surveillance has addressed concerns from rodent studies suggesting osteosarcoma risk, though clinical incidence remains exceedingly rare. Renal function and serum calcium should be assessed periodically to mitigate nephrolithiasis and hypercalciuria.
Emerging Research and Future Directions
Advances in molecular biology, imaging, and biomaterials are driving novel approaches to optimize PTH-based therapies. Efforts to develop depot formulations, oral PTH analogs, and peptides with biased agonism aim to enhance patient compliance and selectively amplify anabolic over catabolic signaling. Gene-editing tools and single-cell transcriptomics offer unprecedented insights into the heterogeneity of osteogenic cell populations and their response to PTH.
Stem cell–based strategies combined with PTH modulation hold promise for accelerating bone repair in complex fractures and skeletal defects. Additionally, elucidation of cross-talk between PTH signaling and pathways such as Wnt/β-catenin, sclerostin inhibition, and mechanotransduction will refine targeted interventions. Ultimately, precision medicine approaches that integrate genetic profiling, biomarker assessment, and individualized dosing regimens are poised to transform the management of metabolic bone disorders and improve clinical outcomes.