The intricate relationship between the endocrine and skeletal systems reveals how disturbances in thyroid function can profoundly affect bone health. This article examines the mechanisms linking thyroid disorders to changes in bone density, highlights clinical implications, and explores strategies for prevention and management.
Thyroid Hormones and Bone Physiology
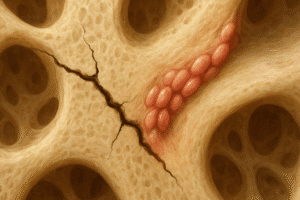
Thyroid hormones play a pivotal role in regulating bone remodeling, a continuous process orchestrated by two main cell types: osteoblasts, responsible for bone formation, and osteoclasts, which drive bone resorption. Under normal conditions, a tightly controlled balance ensures structural integrity. The primary hormones involved include triiodothyronine (T3) and thyroxine (T4), both of which influence cellular activity in bone tissue.
Mechanisms of Action
- T3 binds nuclear receptors in bone cells, accelerating osteoblast differentiation and enhancing osteoclast survival.
- Excess thyroid hormones increase the production of RANKL (receptor activator of nuclear factor kappa-Β ligand), tipping the scale toward resorption.
- TSH (thyroid-stimulating hormone) itself appears to have a protective effect on bone by directly inhibiting osteoclast formation.
- Thyroid hormones modulate calcium homeostasis by affecting intestinal absorption and renal excretion.
Normal Versus Pathological States
In euthyroid individuals, thyroid secretion aligns precisely with metabolic demands, ensuring bone mineral density is maintained within healthy ranges. When dysregulation occurs, either via hyperthyroidism or hypothyroidism, the equilibrium is disrupted:
- Hyperthyroidism accelerates the remodeling cycle, often leading to a net loss of mineralized matrix.
- Hypothyroidism slows down turnover, potentially causing increased bone mass but compromised microarchitecture and quality.
Impact of Hyperthyroidism on Bone Density
Hyperthyroidism is characterized by excessive production of thyroid hormones, commonly due to Graves’ disease or toxic nodular goiter. Elevated T3 and T4 levels stimulate osteoclastic activity, shortening the bone remodeling cycle and reducing the time available for mineralization.
Clinical Consequences
- Accelerated bone loss, particularly in cortical bone, increases fracture risk.
- Postmenopausal women are especially susceptible, as estrogen deficiency compounds thyroid-induced resorption.
- Long-standing untreated hyperthyroidism may lead to secondary osteoporosis.
Diagnostic Markers
Healthcare providers monitor several parameters:
- Serum TSH – typically suppressed in overt hyperthyroidism.
- T3 and T4 levels – confirm hormonal excess.
- Bone turnover markers – such as serum C-terminal telopeptide and osteocalcin.
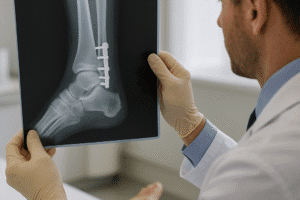
- Dual-energy X-ray absorptiometry (DEXA) – quantifies bone mineral density at key sites.
Effects of Hypothyroidism on Skeletal Integrity
Hypothyroidism results from insufficient thyroid hormone production, most often due to chronic autoimmune thyroiditis or iatrogenic factors. Reduced T3 and T4 concentrations slow osteoblastic and osteoclastic activity, leading to an accumulation of older bone that may be structurally inferior.
Bone Quality Versus Quantity
While hypothyroid patients can exhibit normal or even increased bone mass, the delayed remodeling impairs microarchitecture:
- Trabecular connectivity may weaken, heightening fracture susceptibility despite preserved density.
- Bone stiffness and elastic modulus are altered, affecting the bone’s ability to absorb impact forces.
Clinical Presentation and Diagnosis
- Patients often report joint stiffness and muscle aches, which can mask underlying bone fragility.
- Laboratory tests reveal elevated TSH and low free T4 levels.
- Bone quality assessment may require high-resolution peripheral quantitative computed tomography (HR-pQCT).
Strategies for Prevention and Management
Effective management of thyroid-related bone loss hinges on early detection, restoration of euthyroid state, and targeted bone-protective measures.
Restoring Thyroid Balance
- Antithyroid drugs (e.g., methimazole) or radioactive iodine therapy for hyperthyroidism.
- Levothyroxine replacement in hypothyroid patients, with careful dose titration to avoid overtreatment.
Bone-Directed Therapies
When bone density falls below critical thresholds or fractures occur, adjunct treatments may be indicated:
- Bisphosphonates inhibit osteoclast-mediated resorption, preserving bone mass.
- Selective estrogen receptor modulators (SERMs) can mimic estrogen’s protective effects in postmenopausal women.
- Denosumab, a monoclonal antibody against RANKL, offers a potent alternative for high-risk individuals.
- Calcium and vitamin D supplementation support mineralization and improve overall bone health.
Lifestyle Interventions and Monitoring
A holistic approach encompasses nutrition, exercise, and regular bone surveillance.
Nutrition and Supplementation
- Ensure adequate dietary calcium (1,000–1,200 mg/day) from dairy products, leafy greens, and fortified foods.
- Maintain optimal vitamin D status (serum 25-hydroxyvitamin D ≥ 30 ng/mL) through sunlight exposure and supplements.
- Incorporate protein-rich sources to support collagen matrix synthesis.
Physical Activity
Weight-bearing and resistance exercises stimulate bone formation and improve muscle strength, reducing fall risk:
- Brisk walking, jogging, or stair climbing for at least 30 minutes most days.
- Resistance training using free weights or resistance bands two to three times per week.
- Balance and flexibility routines, such as yoga or tai chi, to prevent falls.
Regular Assessment
- Periodic DEXA scans, particularly in patients with prolonged thyroid dysfunction.
- Monitoring of bone turnover markers to gauge response to therapy.
- Routine evaluation of thyroid function tests to maintain euthyroid status.