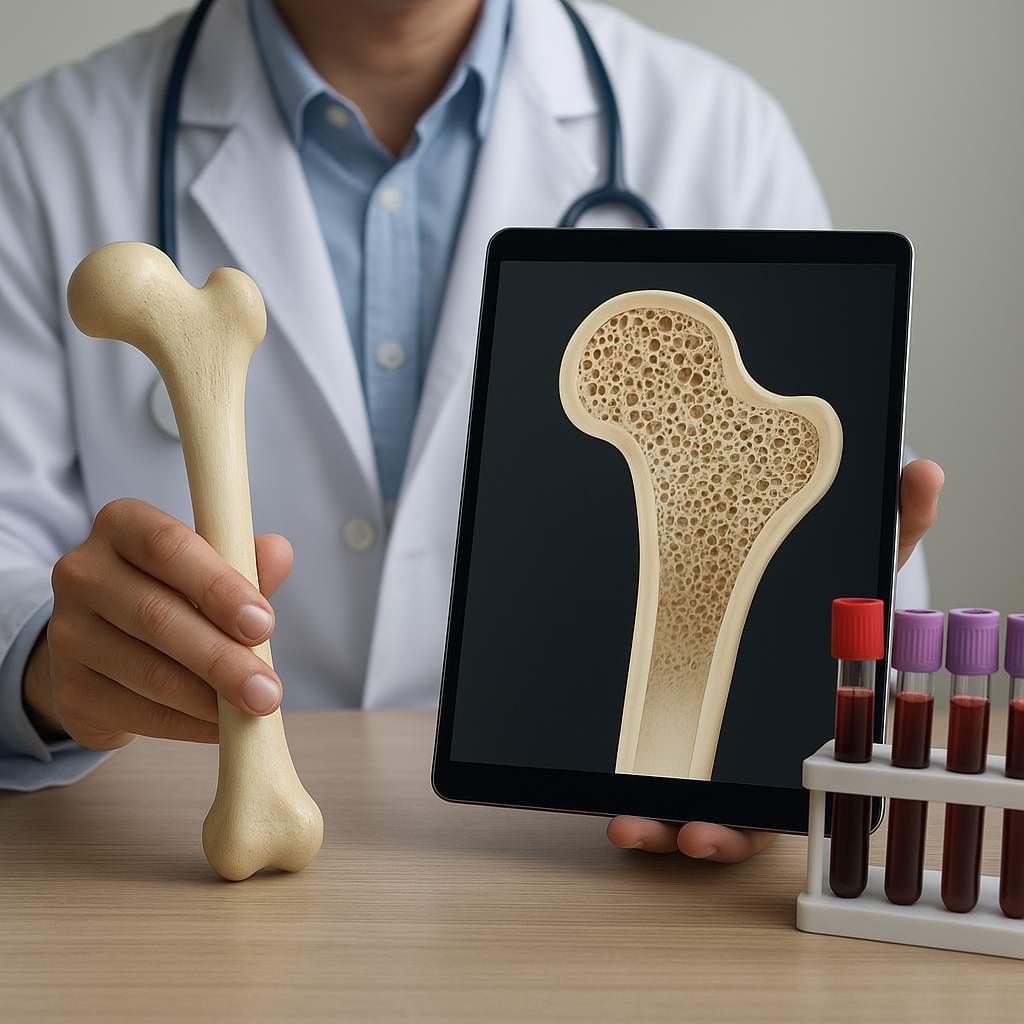
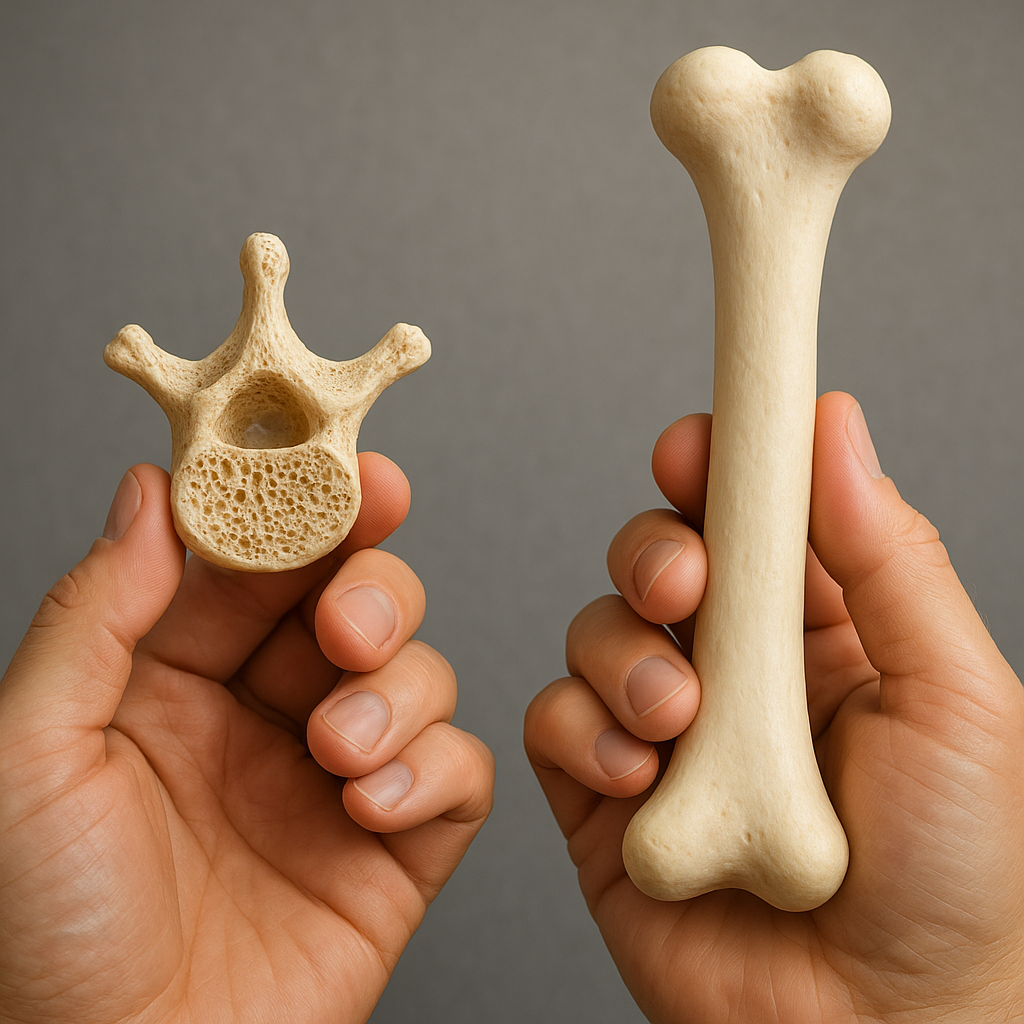
The intricate interplay between the skeletal system and the endocrine network ensures proper bone strength, density, and integrity. Disruptions in hormonal signals can lead to altered bone remodeling, predisposing individuals to fractures and chronic skeletal diseases. This article delves into the mechanisms by which endocrine factors regulate bone metabolism, explores common disorders that compromise skeletal health, reviews current diagnostic strategies, and highlights emerging therapeutic approaches aimed at restoring bone homeostasis.
Hormonal Regulation of Bone Metabolism
Bone undergoes continuous renewal through the balanced activities of osteoblasts (bone-forming cells) and osteoclasts (bone-resorbing cells). Endocrine factors orchestrate these opposing processes by modulating cellular differentiation, proliferation, and function.
Key Hormones and Their Actions
- Parathyroid hormone (PTH): Elevates serum calcium by stimulating osteoclast activity indirectly via release of RANKL from osteoblasts.
- Calcitonin: Secreted by thyroid parafollicular cells, directly inhibits osteoclast resorption and lowers blood calcium.
- Vitamin D (calcitriol): Enhances intestinal calcium absorption and promotes normal mineralization by facilitating osteoblast maturation.
- Estrogen: Suppresses bone resorption by downregulating cytokines that activate osteoclasts and upregulating osteoprotegerin.
- Testosterone: Stimulates periosteal bone formation and indirectly supports osteoblastic activity via aromatization to estrogen.
- Glucocorticoids: When in excess, induce apoptosis of osteoblasts and osteocytes, reduce intestinal calcium uptake, and impair gonadal steroid production.
Common Endocrine Disorders Affecting Bone Health
Disruptions in endocrine glands or hormone synthesis produce systemic effects, many of which have direct consequences on skeletal metabolism.
Hyperparathyroidism
Excess PTH secretion leads to increased bone turnover, characterized by cortical thinning and subperiosteal bone resorption. Primary hyperparathyroidism often presents with bone pain, nephrolithiasis, and osteitis fibrosa cystica.
Hypoparathyroidism
Insufficient PTH reduces bone remodeling rates and results in dense but brittle bones. Patients may experience hypocalcemia, tetany, and neuromuscular irritability.
Thyroid Disorders
- Hyperthyroidism accelerates bone remodeling, shortening the bone formation phase and increasing fracture risk.
- Hypothyroidism slows bone turnover, potentially causing osteosclerosis but with underlying mechanical weakness.
Diabetes Mellitus
Both type 1 and type 2 diabetes impact bone quality. Chronic hyperglycemia leads to advanced glycation end-products in collagen, reducing bone toughness and increasing fragility.
Cushing’s Syndrome
Excess endogenous or exogenous glucocorticoids suppress gonadal hormones, inhibit osteoblast function, and upregulate apoptosis of bone cells, resulting in rapid bone loss, particularly trabecular bone.
Hypogonadism
Low estrogen or testosterone levels diminish the protective effects on bone. Men and women with premature ovarian failure, androgen deprivation therapy, or pituitary disorders display reduced bone density and heightened fracture risk.
Diagnostic Approaches and Biomarkers
Assessment of bone health in endocrine disorders requires a combination of imaging, laboratory assays, and clinical evaluation to detect early changes and guide management.
Bone Mineral Density (BMD) Measurements
- Dual-energy X-ray absorptiometry (DXA): Gold standard for diagnosing osteopenia and osteoporosis, provides T-scores and Z-scores.
- Quantitative computed tomography (QCT): Offers volumetric analysis, better distinguishing cortical from trabecular compartments.
Biochemical Markers of Bone Turnover
- Formation markers: serum osteocalcin, bone-specific alkaline phosphatase.
- Resorption markers: urinary N-telopeptide (NTX), C-telopeptide (CTX), deoxypyridinoline.
Hormone Assays
- PTH and vitamin D metabolites to evaluate calcium homeostasis.
- Thyroid-stimulating hormone (TSH) and free T4 for thyroid status.
- Cortisol levels or dexamethasone suppression test for suspected Cushing’s syndrome.
- Sex steroid profiles in hypogonadism or androgen deprivation therapy contexts.
Therapeutic Strategies and Future Directions
Effective management of bone involvement in endocrine disorders encompasses both hormone normalization and direct bone-targeted therapies.
Hormone Replacement and Modulation
- PTH analogs (teriparatide) for severe osteoporosis linked to hypoparathyroidism or glucocorticoid use.
- Calcimimetics (cinacalcet) in primary hyperparathyroidism to reduce PTH secretion.
- Thyroid hormone titration to maintain euthyroid status and prevent bone loss.
- Sex steroid replacement (estrogen, testosterone) in hypogonadal patients to restore bone protective effects.
Antiresorptive and Bone-Forming Agents
- Bisphosphonates: Inhibit osteoclast activity, first-line in glucocorticoid-induced and postmenopausal osteoporosis.
- Denosumab: Monoclonal antibody against RANKL, reduces bone resorption and fracture rates.
- Sclerostin inhibitors: Promote bone formation by antagonizing an osteocyte-derived inhibitor of Wnt signaling.
Emerging Therapies and Research Frontiers
Advances in genomics and molecular biology have identified novel targets for bone anabolism. Therapies under investigation include:
- Selective androgen receptor modulators (SARMs) that enhance bone formation without undesirable soft tissue effects.
- Gene therapy approaches to correct mutations in PTH receptor or collagen genes.
- MicroRNA-based regulators of osteoblast differentiation and function.
Lifestyle and Nutritional Interventions
- Optimal dietary calcium and vitamin D intake to support mineralization.
- Weight-bearing and resistance exercise to stimulate mechanical loading and bone formation.
- Smoking cessation and moderation of alcohol consumption to minimize bone loss.